Combining perio-restorative protocols to maximize function
This article describes a team approach for periodontal and restorative treatment intended to produce a predictable, biologically sound outcome that preserves more supporting bone and restores carious and broken down teeth. The goal of periodontal treatment, when performed in conjunction with restorative dentistry, is to provide restorative dentists with a high percentage of tooth structure that allows for a supragingival margin. An equally important goal is to ensure that an adequate thickness of connective tissue exists to create an environment more resistant to trauma and inflammation. The team approach consists of a restorative phase and a surgical phase. The restorative phase involves preparation with complete caries removal, adhesive core buildups, and provisionalization. The surgical phase involves biologic shaping of the roots and judicious osseous resection. Case studies are used to demonstrate the team approach. More about the team work in the course Perio-restorative protocols: team-based approach.
Over the years, restorative materials have become so advanced that successful periodontal treatment depends greatly on the work of the restorative dentist. The advent of the adhesive core buildup and provisionals gives the periodontist vertical access to many areas on the tooth surface that might cause periodontal breakdown. It is essential that the restorative dentist place a core buildup prior to periodontal correction. This step allows the periodontist to assign individual tooth prognoses, determine the apical extent of caries (and thus establish a definitive margin before a bone/restorative relationship is developed), and establish complete access for unimpeded treatment. If the core is not completed prior to surgery, there would be no way for the periodontist to determine where the soft tissue and bone should be positioned. If surgery is performed prior to caries removal, core buildups, and provisionalization, the periodontist would, at best, be making an educated guess as to the necessary amount of bone removal. At worst, the periodontist would have no idea how much or how little bone had to be removed and could not even be sure as to which teeth were salvageable. Performing adhesive core buildups enables clinicians to facilitate thorough caries removal, seal dentinal tubules prior to the definitive restoration, provide ideal preparation form, eliminate undercuts in the preparation, increase provisional retention, allow for a uniform thickness of definitive restorative material, minimize distortion or tearing of impressions, and provide the biologic periodontal surgical template.
Biologic shaping
Biologic shaping is an adjunct to conventional crown lengthening. Conventional crown lengthening uses the existing margins of an old restoration or the cementoenamel junction (CEJ) of a non-restored tooth to determine the amount of bone removal necessary to establish adequate space for the biologic width. Creating proper space for the biologic width ensures that a new margin will not impinge upon the periodontal complex and reduces the likelihood of future inflammation. At times, a significant amount of bone must be removed, which can weaken the stability of the tooth or create weakened and vulnerable furcation areas. As more bone is removed from the furcation, the likelihood of future maintenance problems increases. As a result, it is critical to preserve as much bone as possible to support the tooth, especially in the furcation area. Biologic shaping moves the restorative margin away from the bone, minimizing the amount by which the crown must be lengthened to move the bone away from the restorative margin. Table 1 lists reasons, based on the authors’ experience, when biologic shaping might be necessary.
This article examines requirements for successful treatment using a team approach, based on a series of comprehensive periodontal and restorative cases. It will be apparent when doing combined periodontal and restorative treatment that the restorative dentist’s knowledge of materials and biology is paramount to the long-term success of these cases.
Responsibilities of the periodontists
When treating combined periodontal and restorative cases, the periodontist must create a final margin location (either supragingival or just into the sulcus), improve tissue health to guarantee an ideal impression, and provide an abundance of dense, thick connective tissue bound to the root surface and bone to protect the underlying periodontal support.
This abundance of tissue is essential for taking impressions and placing final restorations, since restorations alter the environment and increase the likelihood of inflammation, while a mucosal margin can remain inflammation-free when it is adjacent to a non-restored natural tooth. For esthetic surgical procedures, the periodontist must provide ideal clinical anterior crown length so that the restorative dentist can provide patients with the highest level of esthetic treatment. The periodontist also must make every attempt to avoid black triangles when carrying out surgical procedures and support the restorative dentist by motivating patients to accept the comprehensive treatment plan.
Responsibilities of the restorative dentist
As part of the team approach, the restorative dentist must remove all caries and place core buildups, which provide landmarks that will allow the periodontist to establish the proper location for margin placement. Provisionals must be placed wherever an old crown is to be replaced or decay might impede the location of the final margin. These provisionals will provide the surgeon with vertical access so that all root surface irregularities can be treated and harmony can be created between bone and tooth surface. At four weeks, the provisionals must be relined or remade to provide ideal fit and the proper relationship to the new soft tissue margin. The final restoration must have proper contours and perfect marginal fit to enable long-term maintenance.
Finally, the restorative dentist must support the periodontist by motivating the patient to proceed with proper comprehensive care.
Comprehensive periodontal and restorative procedures
All previous restorative materials and decay should be removed. A core buildup of composite bonded resin should be placed (where necessary) to add volume to the teeth. The core helps to determine where the final margin of the new restoration will be placed. Acrylic provisionals should be luted. The authors recommend using Durelon (3M ESPE) as a temporary cement, due to its anti-microbial properties and ability to help decrease sensitivity. Provisional restorations must be removed at the time of surgery to improve access.
The roots must be shaped and the old margins removed; also, cervical enamel projections must be reduced or eliminated. The ideal restorative emergence profile (flat is better than convex contours) should be established; diamond burs are recommended for this process. Any reverse architecture should be corrected; where biologic width violation is anticipated, bone removal might be necessary. If the surgical site has insufficient keratinized tissue, the connective tissue thickness must be augmented, which will make the marginal tissues less prone to inflammation and protect the supporting bone. In addition, the connective tissue protects underlying periodontal tissues from irritation by impression materials and cementation. Once the flaps are adapted and sutured, liquid potassium oxalate should be used to help decrease postsurgical sensitivity. The liquid is applied to the root surface for 45–60 seconds and lightly air-dried. This step should be repeated two or three times. The provisional prosthesis should be secured with a polycarboxylate cement such as Tylok (Dentsply Caulk) or Durelon. Both of these cements have an antimicrobial effect due to the zinc oxide present in their formulations. Other polycarboxylate cements can be used depending on the operator’s comfort level.
Home care instructions include rinsing with chlorhexidine twice daily (morning and evening) and brushing with a prescription, high concentration fluoride toothpaste at bedtime to help decrease thermal sensitivity. After meals, the patient should rinse with water to remove any food particles. If the patient prefers an over-the-counter mouthrinse instead of water, the authors recommend Listerine (Johnson & Johnson Healthcare Products) due to its demonstrated anti-gingivitis properties.
Table 1. Reasons for biologic shaping.
Replacing or supplementing the current indications for clinical crown lengthening
Minimizing ostectomy
Facilitating supragingival or just slightly intrasulcular margins to preserve the biologic width
Eliminating developmental grooves
Eliminating previous subgingival restorative margins
Reducing or eliminating furcation anatomy, thus facilitating margin placement
Allowing supragingival or intrasulcular impression techniques
Removing all CEJs
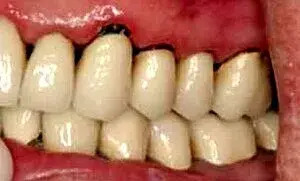 Fig. 1. A preoperative view of leaking crowns.
Fig. 1. A preoperative view of leaking crowns.
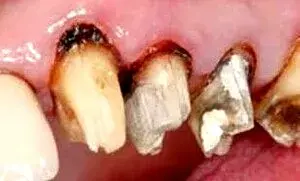 Fig. 2. Caries found under existing restorations.
Fig. 2. Caries found under existing restorations.
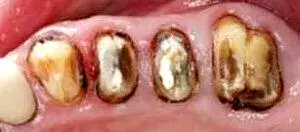 Fig. 3. An occlusal view after the removal of old crowns.
Fig. 3. An occlusal view after the removal of old crowns.
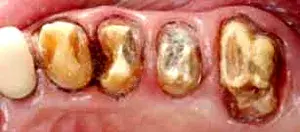 Fig. 4. A patient after complete caries removal.
Fig. 4. A patient after complete caries removal.
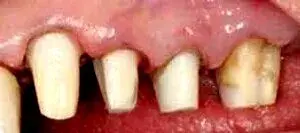 Fig. 5. Adhesive core buildups bonded in place.
Fig. 5. Adhesive core buildups bonded in place.
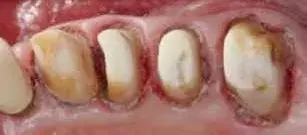 Fig. 6. An occlusal view of the adhesive cores in Figure 5.
Fig. 6. An occlusal view of the adhesive cores in Figure 5.
When the provisionals are remade or relined at four weeks, there should be 1 mm between the provisional and soft tissue margins, which will allow the biologic width to mature in a coronal direction. No preparation or refining of tooth surfaces should be performed at this time. At 14 weeks, chamfer margins are placed just coronal to the gingival collar and impressions are taken. When endodontics are required, the new margin can be placed within the sulcus. The periodontist’s actions should facilitate hygiene and maintenance procedures.
Before the periodontist even treats the patient, the restorative dentist must perform caries removal and place core buildups and provisional crowns. Patients often have existing restorations that are undermined by recurrent decay (Fig. 1–3). All caries must be completely removed without concern for extending the preparation subgingivally (Fig. 4). Retraction cords are used to facilitate isolation and removed after the adhesive cores are completed (Fig. 5 and 6). At that point, biologic, esthetic, and functional determinants can be established. The fixed provisional restorations not only allow dentists to test esthetic and occlusal hypotheses, they also can be removed to provide 360 degree access (Fig. 7 and 8), which allows the periodontist to perform crown lengthening and biologic shaping without impedance.
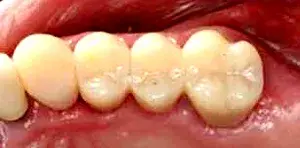 Fig. 7. An occlusal view of the cemented fixed provisional restoration.
Fig. 7. An occlusal view of the cemented fixed provisional restoration.
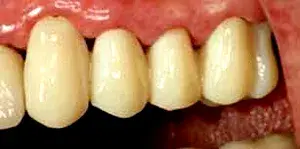 Fig. 8. An anterior view of the provisional restoration in Figure 7.
Fig. 8. An anterior view of the provisional restoration in Figure 7.
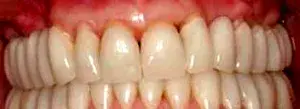 Fig. 9. The provisional restoration is relined 1 mm coronal to the tissue margin.
Fig. 9. The provisional restoration is relined 1 mm coronal to the tissue margin.
Four weeks after periodontal correction, the provisional restoration in the illustrated case is relined 1 mm shy of (or coronal to) the soft tissue margin (Fig. 9). The provisional could have been entirely remade, but nothing more than a simple reline was necessary. There is still no defined restorative margin on the tooth. The biologic shaping has completely removed any restorative margin and all undercuts from bone to the occlusal/incisal surface. From an occlusal view, one sees only a perfectly smooth tube of tooth structure coming through the soft tissues.
Case report No. 1
The patient came to the periodontist with provisionals already in place (Fig. 10). Removing the provisionals gives the periodontist vertical access to all interproximal areas (Fig. 11). If crown lengthening is done prior to provisionalization, the periodontist’s access is severely impaired. Split-thickness flap reflection allows for easy visualization of the core-to-bone relationship and demonstrates that the periodontist has ideal working conditions for performing a treatment that will produce a stable periodontal environment (Fig. 12). The periodontist started by removing all CEJs and irregularities on the root surfaces. Most importantly, the old margins of the restorations were removed, creating a root surface free from any landmarks that dictate bone removal to provide space for the biologic width. A C847-016 bur (Axis Dental) was used initially for tooth surface contouring (Fig. 13).
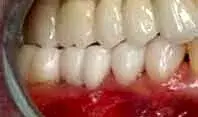 Fig. 10. A patient after caries removal, core buildup, and provisionalization of the mandibular right posterior area.
Fig. 10. A patient after caries removal, core buildup, and provisionalization of the mandibular right posterior area.
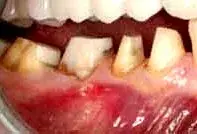 Fig. 11. The patient in Figure 10, following the removal of provisionals.
Fig. 11. The patient in Figure 10, following the removal of provisionals.
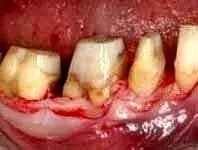 Fig. 12. Reflection of a split thickness.
Fig. 12. Reflection of a split thickness.
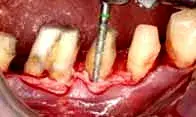 Fig. 13. The patient in Figure 10, following the removal of CEJs, old restorative margins, and root surface irregularities.
Fig. 13. The patient in Figure 10, following the removal of CEJs, old restorative margins, and root surface irregularities.
The periosteum was reflected from the bone to allow for osseous contouring. A C801L-023 bur (Axis Dental) was used for the critical step of creating a parabolic architecture for ideal approximation of soft tissue over bone (Fig. 14). Using a super fine bur (F847-016, Axis Dental), additional contouring and refining was performed to create a smooth root surface (Fig. 15). After biologic shaping and osseous contouring, there were no undercuts in the preparations and the bone demonstrated positive architecture (Fig. 16). With the periosteum repositioned over the bone, connective tissue taken from the palate was sutured in place to increase the support and protection for the underlying periodontal foundation. The authors believe that connective tissue is the key to long-term maintenance of periodontal restorative cases, because it has very few blood vessels and dense, thick connective tissue (Fig. 17). Suturing should position the tissue just coronal to the bone so that the patient experiences minimal discomfort when attempting to achieve primary closure. The connective tissue graft was covered by the overlying flap and 5-0 chromic gut sutures were used to close the buccal flap to the lingual flap (Fig. 18). The occlusal view showed barreled-in furcations. Overhanging tooth structure and all heights of contour were removed from bone level to the occlusal table of the tooth (Fig. 19). The final restorations consisted of an all-ceramic crown on tooth No. 28 and porcelain-fused-to-gold crowns on teeth No. 29–32. It should be noted that the furcal contours of the restorations mimic the underlying tooth structure, which was prepared at the time of surgery (Fig. 20). No heights of contour were placed and the furcations were barreled in all the way to the occlusal surfaces. The soft tissue-to-tooth interface was ideal. The patient was placed on a three-month alternating recall schedule between the restorative dentist and periodontist and has not demonstrated any further break-down since completion of treatment.
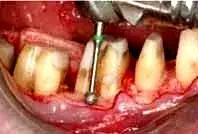 Fig. 14. The patient in Figure 10, after the periosteum is reflected for osseous contouring.
Fig. 14. The patient in Figure 10, after the periosteum is reflected for osseous contouring.
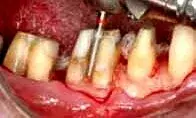 Fig. 15. The patient in Figure 10, after a super fine bur is used for additional contouring of the tooth surface.
Fig. 15. The patient in Figure 10, after a super fine bur is used for additional contouring of the tooth surface.
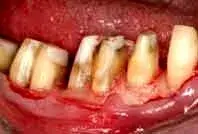 Fig. 16. The patient in Figure 10, after biologic shaping and osseous contouring.
Fig. 16. The patient in Figure 10, after biologic shaping and osseous contouring.
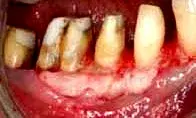 Fig. 17. With the periosteum repositioned over the bone, palatal connective tissue is sutured in place.
Fig. 17. With the periosteum repositioned over the bone, palatal connective tissue is sutured in place.
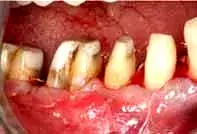 Fig. 18. A connective tissue graft is covered by an overlying flap.
Fig. 18. A connective tissue graft is covered by an overlying flap.
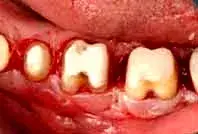 Fig. 19. An occlusal view shows barreled-in furcations.
Fig. 19. An occlusal view shows barreled-in furcations.
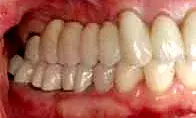 Fig. 20. The furcation contours of the final restorations mimic the underlying tooth structure.
Fig. 20. The furcation contours of the final restorations mimic the underlying tooth structure.
Case report No. 2
As is often the case, caries control and provisionalization occurred prior to periodontal surgery (Fig. 21). The provisionals were removed to allow the periodontist unimpeded vertical access (Fig. 22). Reflecting the soft tissue revealed a mesial concavity on tooth No. 12, with associated calculus present (Fig. 23). Removing the mesial concavity made it possible to place a restorative margin just coronal to the gingival collar at 12 weeks. Removing the concavity gives the hygienist and patient easy access to plaque, calculus, and biofilm for long-term maintenance (Fig. 24). Once the restorations have been completed, the patient will be placed on a three-month alternating recall schedule between the restorative dentist and the periodontist.
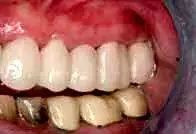 Fig. 21. A patient with provisionals placed in advance of periodontal correction.
Fig. 21. A patient with provisionals placed in advance of periodontal correction.
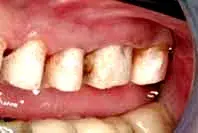 Fig. 22. The patient in Figure 21, after the removal of provisionals.
Fig. 22. The patient in Figure 21, after the removal of provisionals.
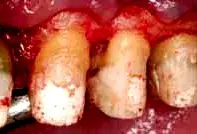 Fig. 23. Reflected tissue shows a mesial concavity on tooth No. 12, with associated calculus.
Fig. 23. Reflected tissue shows a mesial concavity on tooth No. 12, with associated calculus.
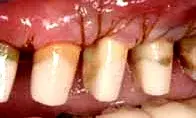 Fig. 24. The patient in Figure 21, following removal of the mesial concavity.
Fig. 24. The patient in Figure 21, following removal of the mesial concavity.
Case report No. 3
In this case, teeth No. 19 and 20 were treated using a periodontal-restorative approach. Caries was removed and the teeth were provisionalized (Fig. 25). After the provisionals were removed, the soft tissues showed ideal health, which can occur only when provisionals are perfectly contoured and fitted. The minimal vertical probing depth in the furcation can be deceptive. When restoring molars with existing restorations, it is critical to evaluate not only the vertical probing, but the horizontal component of the furcation as well (Fig. 26). While vertical probing was minimal, the horizontal probing depth demonstrated significant furcation breakdown (Fig. 27). The furcation was removed and any furcation roof was eliminated to create an environment for a crown that fit well with no areas where plaque and calculus could accumulate. After osseous recontouring, the periosteum was positioned in place (Fig. 28). The tissue was positioned just coronal to the bone to allow for ideal development of a new biologic width. To promote more rapid healing and decrease patient discomfort, one must always attempt to gain primary closure of the soft tissue when suturing flaps. Due to the location of pulp chambers, endodontic treatment is not usually necessary when barreling out furcations. (Fig. 29). The goal of the periodontist is to provide the restorative dentist with a tooth surface upon which she or he can place a margin just coronal to the gingival collar. A feldspathic porcelain crown with proper contours in the furcation area allows the patient and hygienist to perform long-term maintenance.
In the present case, the porcelain furcation could have been carried to the occlusal surface to prevent any unnecessary height of contour in the final restoration (Fig. 30). A one-year postoperative radiograph verified that the pulp of tooth No. 19 was healthy and that there was no indication for endodontic treatment (Fig. 31).
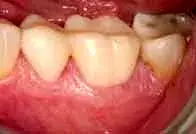 Fig. 25. A patient with provisionals on teeth No. 19 and 20 in advance of periodontal correction.
Fig. 25. A patient with provisionals on teeth No. 19 and 20 in advance of periodontal correction.
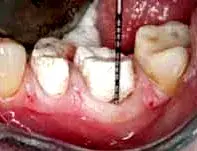 Fig. 26. The patient in Figure 25, with minimal vertical probing depth in the furcation.
Fig. 26. The patient in Figure 25, with minimal vertical probing depth in the furcation.
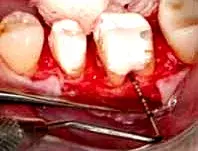 Fig. 27. The horizontal probing depth demonstrates significant furcation breakdown.
Fig. 27. The horizontal probing depth demonstrates significant furcation breakdown.
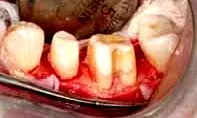 Fig. 28. The patient in Figure 25, following complete removal of the furcal roof and any heights of contour.
Fig. 28. The patient in Figure 25, following complete removal of the furcal roof and any heights of contour.
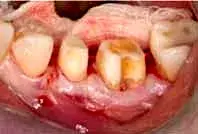 Fig. 29. Tissue positioned just coronal to bone for development of a new biologic width.
Fig. 29. Tissue positioned just coronal to bone for development of a new biologic width.
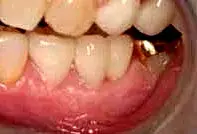 Fig. 30. The final restorations, with equigingival margin placement.
Fig. 30. The final restorations, with equigingival margin placement.
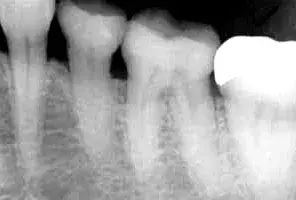 Fig. 31. Tooth No. 19, as seen in a postoperative radiograph of the patient in Figure 25.
Fig. 31. Tooth No. 19, as seen in a postoperative radiograph of the patient in Figure 25.
Summary
Many of today’s patients have restorative needs that often require the replacement of existing dentistry. Often, caries removal and the establishment of a new restorative margin places the anticipated new restorations in an apical or more subgingival position, which presents a number of biologic and mechanical problems that could downgrade the long-term prognosis of both the periodontal health and the restorations. In order to achieve superior restorative results, periodontal corrective procedures are necessary to return the foundation to a healthy state. Traditionally, crown lengthening was indicated for deep subgingival margins—not only to facilitate impression taking, but to correct biologic width impingement. Attempting to take impressions or to cement or bond restorations in this septic environment, and expecting good results, is unrealistic. A combined periodontal/restorative protocol termed biologic shaping has been documented to address these issues with predictable, reproducible clinical precision and long-term success.
Disclaimer
The authors have no relationship with any of the manufacturers mentioned in this article.
Author information
Dr. Tucker is in private practice limited to periodontics and implant surgery in Seattle, Washington. He is a faculty member at the Pikos Implant Institute, Palm Harbor, Florida.
Dr. Melker is in private practice limited to periodontics in Clearwater, FL.
Dr. Chasolen is in private practice limited to prosthodontics in Sarasota, FL. He is also an affiliate clinical instructor, Department of Graduate Prosthodontics, University of Florida School of Dentistry, Gainesville.
References
Vaidyanathan TK, Vaidyanathan J. Recent advances in the theory and mechanism of adhesive resin bonding to dentin: A critical review. J Biomed Mater Res Part B Appl Biomater 2009; 88(2):558-578.
Strupp WC Jr. Crown & Bridge Update 1999;4(1): 1-7.
DiFebo G, Carnevale G, Sterrantino SF. Treatment of a case of advanced periodontitis: Clinical procedures utilizing the “combined preparation” technique. Int J Periodontics Restorative Dent 1985;5(1):52-62.
Melker DJ, Richardson CR. Root reshaping: An integral component of periodontal surgery. Int J Periodontics Restorative Dent 2001;21(3):296-304.
Strupp WC Jr, Melker DJ. Maximizing aesthetics using a combined periodontal-restorative protocol. Dent Today 2003;22(5):60-69.
Gargiulo AW, Wentz FM, Orban B. Dimensions and relations of the dentogingival junction in humans. J Periodontol 1961;32:261-267.
Vacek JS, Gher ME, Assad DA, Richardson AC, Giambarresi LI. The dimensions of the human dentogingival junction. Int J Periodontics Restorative Dent 1994;14(2):154-165.
Dibart S, Capri D, Kachouh I, Van Dyke T, Nunn ME. Crown lengthening in mandibular molars: A 5-year retrospective radiographic analysis. J Periodontol 2003;74(6):815-821.
Stetler KJ, Bissada NF. Significance of the width of keratinized gingiva on the periodontal status of teeth with submarginal restorations. J Periodontol 1987;58(10):696-700.
If you enjoyed reading the article and would like to explore the perio-restorative protocols further, we encourage you to enroll in our course by Daniel Melker "Advanced periodontology: surgical protocols".