Features of prosthetics in old age. Psychological preparation
According to WHO data, the share of elderly people in the total population of developed countries is increasing every year, and their number among patients of dentists is correspondingly growing. Studies have established that among elderly people there is a high rate of complete absence of teeth.
Causes of complete edentia
caries and its complications,
periodontal diseases,
injuries,
primary congenital adentia, the rarest of the listed causes.
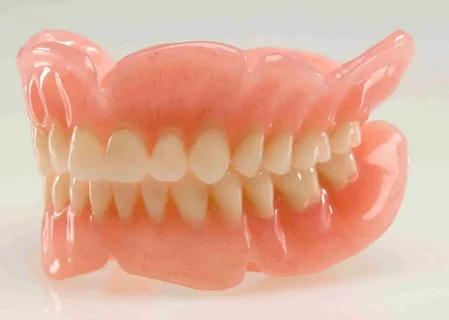
Rice. 1. Complete removable dentures.
The complete absence of teeth entails serious consequences for the patient, reduces the quality of his life, and affects the functioning of the body as a whole.
Impaired chewing of food affects the digestion process and causes diseases of the gastrointestinal tract.
Speech impairment causes communication problems for the patient.
Appearance changes as a result of progressive atrophy of the masticatory muscles, which often leads to a disturbance in the psycho-emotional state of an elderly person and a disorder of his psyche.
Dysfunction of the temporomandibular joint develops, and orofacial pain appears.
The doctor is faced with the difficult task of not only providing prosthetics to a patient with complete edentia, but also creating a prosthesis that will completely satisfy the patient and solve functional and aesthetic problems.
Modern dentistry can offer more effective methods for eliminating complete adentia using implants, but this type of orthopedic care is not available to most patients, due to its high cost.
Despite the constant improvement of treatment methods, the introduction of modern technologies in orthopedic treatment for complete edentia, the fixation of complete removable dentures in the mouth only worsens with age. The manufacture of removable dentures requires high professionalism of an orthopedist and dental technician.
Rice. 2. Informing the patient about the upcoming treatment.
The result of prosthetics is determined by the following factors:
anatomical features of the patient’s oral cavity;
professionalism of the team of orthopedic and dental technicians;
psycho-emotional state of the patient;
materials used;
equipment and treatment methods.
In the process of prosthetics for patients with complete absence of teeth, it is necessary to solve a number of problems:
ensure fixation of dentures on toothless jaws;
think over the design of the prosthesis in such a way that it functions synchronously with the masticatory apparatus, ensuring high-quality mechanical processing of food, sound reproduction, and breathing;
determine the individual size and shape of prostheses in order to restore lost facial proportions.
To solve these problems, it is necessary to know the topography of the oral mucosa and toothless jaws.
Psychological preparation of patients
The success of prosthetics with complete edentia directly depends on the psychological state of the patient, which, unfortunately, is rarely taken into account by orthopedic dentists. Scientists have found that before prosthetics, it is important to assess the characteristics of the patient’s psyche, his behavior and reaction. This will help you choose the optimal medical tactics, create positive communication between the patient and the doctor, which will help eliminate negative emotions and will serve as a prevention of complications of orthopedic treatment.

Rice. 3. Positive communication between the doctor and the patient.
In the process of collecting anamnestic data, along with standard questions for an orthopedist, it is worth trying to determine whether the patient has the following problems:
mental illness,
atherosclerosis,
neuropsychiatric disorders,
traumatic brain injuries,
alcoholism.
All elderly patients can be divided into the following groups based on their mental state.
The psycho-emotional state is normal and corresponds to age. Before starting prosthetics, it is important for such patients to explain the plan and purpose of prosthetics, familiarize them with the design, type of prosthesis, problems that may arise during the adaptation stage, and the nuances of caring for prostheses. During the last appointment after applying the prosthesis, it is important to repeat the care recommendations, and it is better to also give a reminder.
Patients with neuropsychic disorders that do not interfere with the choice of the optimal design of dentures, however, require special monitoring for the care of dentures. Handing over a leaflet with recommendations for caring for such patients is a necessity. Family members caring for the elderly patient should also be given instructions on the rules of care.
Patients with pathological requirements for a prosthesis. Before starting prosthetics, it is necessary to agree with them on all the nuances: the treatment plan, the boundaries of the prosthesis, its shape and size, the shade of artificial teeth. It is important to take into account the wishes of the patient, but not to abuse them, to categorically exclude fundamentally incorrect wishes, but to agree with those that will not lead to prosthetic errors.
Patients who have an established diagnosis of mental illness. If possible, their prosthetics are performed in a hospital setting. Recommendations for the care of dentures are transmitted in writing to the patient's relatives.
Psychological preparation for repeated prosthetics
On the eve of repeated prosthetics, the doctor should determine whether the elderly patient has concerns regarding the upcoming prosthetics. This may be caused by problems that the patient encountered during previous treatment:
discomfort under the prosthesis, pain,
burning, itching in the area of the prosthetic bed,
nausea when wearing
hypersalivation,
fatigue of the masticatory muscles.
These complaints may be caused by the following reasons:
unsatisfactory stabilization and fixation of the prosthesis in the oral cavity,
inability to chew food well,
sensory disturbance,
decubital ulcers,
mucosal reaction.
During a conversation with a patient, the doctor needs to find out the patient’s opinion about the reasons for the failure of previous treatment, as well as evaluate behavior, gestures, posture, and facial expressions.

Rice. 4. Creating a comfortable environment at the reception.
The importance of psychological preparation for accelerating adaptation to prostheses
Often, an orthopedic dentist in his practice encounters patients who have serious problems adapting to removable dentures, but this is primarily due to the psychological status of the patient, and not to the design features or technological performance of the prosthesis.
However, in order to establish the true cause of long-term adaptation, it is first necessary to exclude any technological errors that could have occurred at one of the clinical or laboratory stages of creating prostheses, causing a violation of the functional or aesthetic characteristics of the product.
Early, within the first 6-24 hours from the moment of application of the dentures, correction of the bases, fixing elements, checking the occlusion, and, if necessary, additional grinding and polishing of the dentures is very important. If the patient does not notice any improvement, it can be assumed that the cause of the impaired adaptation is not the prosthesis, but mental factors.
Even a well-made prosthesis requires a significant period of time for an elderly person to get used to it. And for patients who have been using removable dentures for a long time, over the years it only becomes more difficult to get used to something new. They develop a strong habit of a certain shape and size of the prosthesis, so that any minor difference makes the new prosthesis as uncomfortable as possible, preventing the patient from adapting to it.
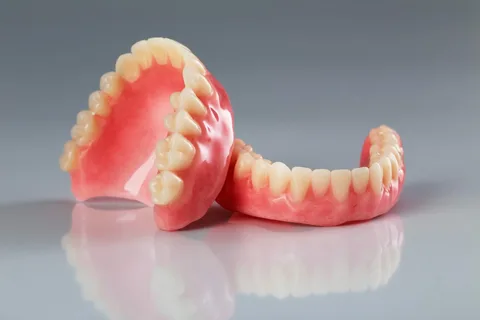
Rice. 5. Ready-made removable dentures.
Such patients are absolutely unable to adapt to a prosthesis, which has even minor design features compared to the previous one. Understanding by an orthopedist of the psychogenic nature of such patient behavior is essential for the success of orthopedic treatment. Of great importance is the doctor’s knowledge of the basics of psychotherapy, namely, sincere interest, the desire to achieve a positive result through joint efforts.
A convincing, calm argument that the manufactured prostheses are not the reason that disrupts adaptation is best suited. Psychotherapy techniques, attention and participation are powerful weapons in the hands of a doctor, when used skillfully, to establish contact and form a positive experience of prosthetics in an elderly patient.