Agreement between Research Diagnostic Criteria for Temporomandibular Disorders and Magnetic Resonance Diagnoses of Temporomandibular disc displacement in a patient population
Abstract
The aim of this work was to evaluate the agreement between the clinical Research Diagnostic Criteria for Temporomandibular Disorders (RDC/TMD) examination and magnetic resonance (MR) findings of temporomandibular joint (TMJ) disc position abnormalities in a sample of clinically symptomatic patients, recruited from a population seeking TMD treatment. Two-hundred and thirty-two TMJs of 116 patients were evaluated to detect disc position abnormalities by means of a standardized clinical assessment according to RDC/TMD guidelines and MR performed blind by a radiologist. The overall kappa value for agreement between clinical examination according to RDC/TMD classification system and MR imaging for assessment of the disc–condyle relationship was fairly good (K = 0.63). The kappa values for the agreement between RDC/TMD and MR diagnosis of disc displacement with reduction (DDR), disc displacement without reduction (DDNR) and normal disk position were 0.69, 0.57, and 0.61, respectively. The observation that clinically predicted cases of DDR and DDNR show good to excellent agreement with MR findings, and the potential MR over-diagnosis of DDR and DDNR in the absence of clinical symptoms, support the usefulness of a standardized examination conducted by a trained investigator in the evaluation of patients with TMD.
Temporomandibular joint (TMJ) disc displacement is one of the most common forms of temporomandibular disorder (TMD). At present, magnetic resonance (MR) is considered the standard of reference for non-invasive diagnosis of TMJ disc displacement, on the basis of studies which compared MR findings with surgical and autopsy specimens, and reported an accuracy of about 90%–95% for detecting disc position abnormalities when both coronal and sagittal images are evaluated.
The assumptionthat a single imagingtest (i.e. MR) allows disease definition may be questionable from a clinical viewpoint. Some recent works pointed out the existence of a significant number of asymptomatic and non-problematic cases with disc position abnormalities that would never be clinically typified as diseased. The use of MR must be reserved for cases in which treatment choice and outcome might be altered by the information thereby gained. Given these premises, it appears logical that the decisional process leading to the choice of a MR examination must be based on the most accurate clinical diagnosis.
A number of studies were conducted to evaluate the accuracy of clinical diagnosis of TMJ disc displacement, but findings are controversial due to the different criteria adopted.
Although the Research Diagnostic Criteria for Temporomandibular Disorders (RDC/TMD) are considered the standard of reference for classification of TMD and for a comparison of diverse studies, providing guidelines and specifications to diagnose disc displacement as well, only a few studies have compared RDC/TMD and MR diagnosis of disc position1. This study, which is part of an ongoing investigation of the predictive value of clinical assessment, attempts to evaluate the agreement between RDC/TMD and MR diagnoses of disc displacement.
There are additional details that you can obtain "Online congress on evidence-based temporomandibular disorders and bruxism treatment".
Materials and methods
Study Sample and Design
Participants were selected from patients presenting during the period January–December 2006 for TMD treatment. One hundred and fifty patients underwent both a clinical assessment according to the RDC/TMD6 and bilateral MR of the TMJs. Thirty-four patients selected for MR were excluded from statistical analysis due to the presence of systemic diseases affecting joint and/or masticatory muscles, such as fibromyalgia or other rheumatic diseases diagnosed according to the American College of Rheumatology criteria. Therefore, a comparison of clinical RDC/TMD and MR TMJ disc position diagnoses was made for 116 patients (88 females, 28 males; mean age 48.6, range 18–65).
The study was carried out in a singleblind fashion, so each patient received a clinical RDC/TMD examination and underwent MR with the clinicians and the radiologist not knowing the result of the other investigation. The two examinations were conducted within 2 weeks of each other, and the patients underwent no treatment during this period. All clinical assessments were performed by the same two trained investigators who performed clinical assessments in accordance to the RDC/TMD guidelines. MR images were interpreted by the same radiologist with expertise in TMJ imaging, who made the diagnosis of disc displacement according to parameters selected from the literature.
RDC/TMD assessment
Clinical assessment was conducted using a standardized clinical protocol including evaluation of patient history, palpation of TMJs, auscultation of joint noises and measurement of mandibular range of motion. According to the guidelines of RDC/TMD6, disc position was categorized as: normal; disc displacement with reduction; disc displacement without reduction (DDR), with or without limited opening. Criteria for inclusion of joints in the different categories were as follows.
RDC/TMD axis I group IIa, diagnosis of DDR:
reciprocal clicking in TMJ (click on both vertical opening and closing that occurs at a point at least 5 mm greater interincisal distance on opening than on closing and is eliminated on protrusive opening) reproducible on two of three consecutive trials; or
clicking in TMJ on both vertical range of motion (either opening or closing) reproducible on two of three consecutive trials, and click during lateral excursion or protrusion reproducible on two of three consecutive trials.
RDC/TMD axis I group IIb, diagnosis of DDNR with limited opening:
history of significant limitation in opening;
maximum unassisted opening 35 mm;
passive stretch increases opening by 4 mm or less over maximum unassisted opening;
contralateral excursion <7 mm and/or uncorrected deviation to ipsilateral side on opening;
absence of joint sounds or presence of joint sounds not meeting criteria for DDR.
RDC/TMD axis I group IIc, diagnosis of DDNR without limited opening:
history of significant limitation of mandibular opening;
maximum unassisted opening >35 mm;
passive stretch increases opening by 5 mm or more over maximum unassisted opening;
contralateral excursion 7 mm;
presence of joint sounds not meeting criteria for DDR.
Magnetic resonance
MR was carried out with a 1.5 Tesla (GE Signa Contour; GE Medical Systems, Buc, France) with a bilateral dedicated circular (8-cm diameter) surface coil for concomitant right and left TMJ study. The investigation protocol provided for a first axial scan ‘‘scout’’ from which were established seven sagittal-oblique slices in a lateral-medial direction and coronal sections deviated obliquely in a postero-anterior direction. Gradient Echo sequences were performed: 2D T1-weighted in sagittal-oblique sections at closed and open mouth and coronal sections at closed mouth (TR = 340 ms, TE = 16 ms, field of view = 15 cm, slice thickness = 3 mm, matrix 256 192) with an interslice gap of 0.5 mm. Sequential bilateral images in both closed mouth and maximum opening mouth positions were made. The latter position was obtained by means of a wooden intermaxillary device at the same opening as measured clinically. The articular disc was directly identified, in sagittal-oblique images, as an area of hypointensity with a biconcave shape above the condylar structure, and its position was categorized according to literature data as follows.
Superior (normal) disc position (N): posterior band of articular disc located above the apex of the condylar head (at 12 o’clock position) in both intercuspal and maximum opening mouth positions.
Disk displacement with reduction (DDR): posterior band of the disc located anteriorly to the condylar head at the closed mouth position, but normal disk condyle relationship established in maximal opening position. Disk displacement without reduction (DDNR): posterior band positioned anteriorly to the condyle either at closed or maximal opening mouth positions.
Statistical analysis
The agreement between the clinical and MR imaging diagnoses was assessed by means of the kappa statistic11. The subcategories of DDNR (with or without limited opening) were grouped together, since no validated MR parameters exist to discriminate between these two conditions. All statistical procedures were performed with the Statistical Package for the Social Sciences (SPSS 11.0, SPSS Inc., Chicago, IL, USA).
Results
MR showed DDR in 82 of the 232 TMJs (35%) and DDNR in 48/232 (21%). A normal superior disc position was diagnosed in 102/232 joints (44%). Clinical RDC/TMD assessment agreed with 60 of the 82 MR-diagnosed DDR, while a normal disc position was clinically diagnosed in the remaining 22 joints. Six joints which received a MR diagnosis of DDNR and 4 presenting a normal disc position were erroneously given a clinical diagnosis of DDR (Table 1).
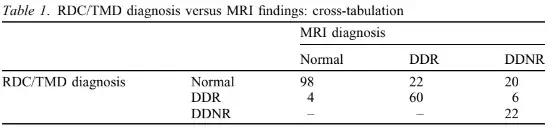
The resulting kappa value for the agreement between RDC/TMD and MR diagnoses of DDR was 0.69 (Table 2).
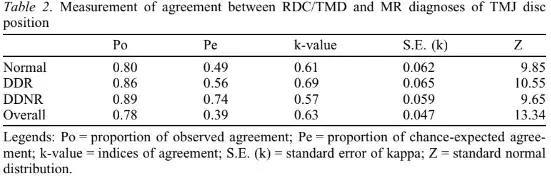
DDNR was clinically diagnosed in 22 out of 48 MR-diagnosed DDNR cases. In 12 of these cases the patient showed limited opening (RDC/TMD axis I group IIb), so it was supposed that they had been intercepted in the acute stage. The other 10 cases did not present a limited opening and had crepitus noises, and the patients’ clinical histories suggested a RDC/TMD axis I group IIc diagnosis. In the other 26 joints which received a MR diagnosis of DDNR, the clinical diagnosis was normal in 20 cases and DDR in 6 joints. The resulting kappa value for the diagnosis of DDNR was 0.57.
A clinical diagnosis of normal disk condyle relationship was established in 140 joints. In 98 of these joints MR confirmed the diagnosis of a normal disc position, in 22 showed a DDR and in 20 a DDNR. A clinical diagnosis of DDR was made in 4 of the 102 joints MR revealed to have a normal superior disc position. The kappa value for the assessment of normal disk-condyle relationship was 0.61. The overall kappa value for agreement between the clinical examination according to the RDC/TMD classification system and MR imaging for the assessment of disk condyle relationships was fairly good (K = 0.63)28.
Discussion
The agreement between clinical and imaging-based diagnoses of disc displacement varies among different studies, ranging from 59% to 90%, and seems to depend mostly upon the diagnostic clinical criteria adopted. Most authors suggest that clinical evaluation does not allow an accurate assessment of the disc concondyle relationship1,10,36, but such observations may be due to MR over-diagnosis (false positive results) rather than clinical under-diagnosis (false negative results). This raises concerns about the role of MR as an appropriate standard of reference for the diagnosis of disk-condyle relationship, and results of different studies are contrasting.
EMSHOFF and RUDISCH10 reported a poor agreement between clinical assessment and MR findings for the diagnosis of DDR (k = 0.13), DDNR (k = 0.33) and normal disc position (k = 0.18), also observing that Clinical Diagnostic Criteria for TMD (CDC/TMD), from which the RDC/TMD classification system was derived, have only a 44% positive predictive value for the diagnosis of DDR7. In a successive paper, the conclusion was made that MR diagnoses cannot be considered dominant for the study of TMJ. This last observation came also from works by YATANI et al. who, despite claiming the poor predictability of historical or clinical findings to diagnose DDNR, suggested that anterior DDR can be diagnosed with considerable accuracy through the use of a clinical examination only.
Divergence between studies is likely to be due to differences in patient recruitment and assessment. To the authors’ present knowledge, the RDC/TMD6, which are recommended as a classification system to allow comparison of diverse studies, have been adopted in only a few studies. In one of these works, an investigation similar to the present study was conducted by one of the authors at his previous academic centre, and some divergences from the other similar papers in the literature had already emerged. A work by BARCLAY et al. reported a high number of clinical false-negative results, which determined a low agreement (53.8%) between clinical RDC/ TMD assessment and MR findings. Such results suggest that MR provided evidence of an abnormal disk–condyle relationship for a number of clinically asymptomatic joints, and confirmed observations from previous MR studies on symptom-free subjects showing disk anteriorization in 33% of subjects with clinically normal, undisturbed jaw function. Contrasting results emerged from a work by WATT-SMITH et al., who carried out arthrotomography and MR in 50 joints of 48 patients with internal derangements undergoing TMJ surgery. The clinical diagnosis of internal derangement was confirmed in every case by imaging and at surgery and, above all, the authors stated that MR over-diagnosed DDNR. In the present investigation, agreement between clinical RDC/TMD examination and MR findings was fairly good (K = 0.63), with disagreement in 22% of cases. Clinical assessment was found to be more accurate than in other studies to detect DDR (K = 0.69). MR confirmed the clinical diagnosis of DDR in 60/70 joints, depicting DDNR (n = 6) and normal disc position (n = 4) in the remaining 10 joints.
The agreement between RDC/TMD and MR diagnoses for DDR was higher than that reported by BARCLAY et al., who found a positive predictive value of 68% for the clinical diagnosis of DDR. The 10 cases of disagreement between clinical and MR findings were due to the presence of click sounds, which erroneously led to a clinical diagnosis of DDR. Such findings lend support to the body of literature suggesting that a click sound may be present in joints with a normal disk–condyle relationship as well as those with DDNR. In line with other investigations, a click sound was not always present in joints with DDR, since 22 of the 42 joints in which MRI showed a DDR were clinically silent.
Taken together, these findings suggest that anamnestic data gathering in accordance with RDC/TMD is of basic importance to improve the accuracy of clinical diagnosis of disc position.
As for DDNR, RDC/TMD assessment allowed prediction of only 22 of the 48 joints with a MR diagnosis of DDNR, of which 12 had a limited range of movement and 10 non-restricted jaw movement. Of the remaining 26 joints which received a MR diagnosis of DDNR, 20 were clinically diagnosed as having a normal disc–condyle relationship and 6 were diagnosed as DDR.
Disagreement between clinical and MR findings was dueto a combination of factors such as the absence of limitation, the misinterpretation of crepitus sounds, whose presence leads to the diagnosis of osteoarthrosis but may be also related to long-term disc displacement, and the concurrent presence of muscle disorders, which often confounds the diagnosis of intrarticular disorders. Such observations are in agreement with other studies and give plausible explanations for the lower agreement between clinical and MR diagnosis of DDNR (K = 0.57). These results suggest some further considerations which may be important in terms of clinical and decision-making impact. While clinical RDC/TMD assessment seems not to be appropriate to detect all cases of DDNR, it is notable that all the clinical diagnoses of DDNR were confirmed by MR. This last observation has huge importance since, in terms of therapeutic perspectives, the absence of false-positive results is very useful in non-life-threatening disorders such as TMD, and DDNR cases identified by means of clinical assessment are probably those most in need of some form of therapy. This consideration has been noted by other authors. As for joints which were clinically diagnosed as having a normal diskcondyle relationship, MR showed a correct disk–condyle relationship in 70% of cases (98/140), but revealed DDR in 22 joints and DDNR in 20 joints. These findings are in agreement with other studies reporting a high variability of disc position in asymptomatic subjects or highly variable symptoms in abnormal subjects. These results give a kappa value of 0.61 for the diagnosis of normal disccondyle relationship.
The overall findings suggest that clinical RDC/TMD assessment agrees well with MR in the diagnosis of TMJ disc position (K = 0.63), but generalization of results and conclusions about clinical implications have to be tempered by some considerations of the study sample. The absence of control asymptomatic subjects makes it impossible to draw strong conclusions about the agreement between clinical and MR findings, and about the specificity of clinical assessment in particular, and may be responsible for divergences between the present investigation and other similar works in the literature.
The study sample was not constituted of all patients seeking TMD treatment, since MR cannot be requested as a routine exam for all patients. This means that information about TMJ disc position gained by clinical assessment alone might have been sufficient in the simplest cases for which MR was not requested and, consequently, that agreement between clinical and MR diagnoses would be even higher if all cases were considered for statistical analysis. The choice to adopt the RDC/TMD classification system was forced by the need for data comparable with those from other similar studies, but the RDC/TMD were never meant to be the most accurate clinical diagnostic criteria. This means that the accuracy of a comprehensive clinical assessment to diagnose disc position might be higher than that reported in the present investigation. Considering these limitations, which seem to prevent the achievement of an even higher rate of agreement between clinical and MR diagnosis, the contrast between the findings of the present investigation and those of previous similar studies appears to be even more striking and worthy of further investigation.
In conclusion, findings from the present investigation suggest that cases of DDR and DDNR that are predicted by clinical RDC/TMD assessment show good to excellent agreement with MR findings. MR diagnosis of disc displacement in the absence of bothersome symptoms suggests over-diagnosis when this is used as the only diagnostic test.
You have the opportunity to gather more in-depth information on TMJ radiodiagnostics in our course.
Acknowledgement. The authors wish to thank Alberto Tregnaghi, MD, who was responsible for magnetic resonance imaging interpretation and diagnosis.
References
Barclay P, Hollender LG, Maravilla KR, Truelove EL. Comparison of clinical and magnetic resonance imaging diagnoses in patients with disk displacement in the temporomandibular joint. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1999: 88: 37–43.
Bertram S, Rudisch A, Innerhofer K, Pumpel E, Grubwieser G, Emshoff R. Diagnosing TMJ internal derangement and osteoarthritis with magnetic resonance imaging. J Am Dent Assoc 2001: 132: 753–761.
Brooks SL, Brand JW, Gibbs SJ, Hollender L, Lurie AG, Omnell KA, Westesson PL, White SC. Imaging of the temporomandibular joint. A position paper of the American Academy of Oral and Maxillofacial Radiology. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1997: 83: 609–618.
Donlon WC, Moon KL. Comparison of magnetic resonance imaging, arthrotomography and clinical and surgical findings in temporomandibular joint internal derangements. Oral Surg Oral Med Oral Pathol 1987: 64: 2–5.
Dworkin SF, Huggins KH, LeResche L, Von Korff M, Howard J, Truelove E, Sommers E. Epidemiology of signs and symptoms in temporomandibular disorders: clinical signs in cases and controls. J Am Dent Assoc 1990: 120: 273–281.
Dworkin SF, Leresche L. Research diagnostic criteria for temporomandibular disorders: review, criteria, examinations and specifications, critique. J Craniomand Disord 1992: 6: 301–355.
Emshoff R, Brandlmaier I, Bosch R, Gerhard S, Rudisch A, Bertram S. Validation of the clinical diagnostic criteria for temporomandibular disorders for the diagnostic subgroup – disc derangement. J Oral Rehabil 2002: 29: 1139–1145.
Emshoff R, Brandlmaier I, Gerhard S, Strobl H, Bertram S, Rudisch A. Magnetic resonance imaging predictors of temporomandibular joint pain. J Am Dent Assoc 2003: 134: 705–714.
Emshoff R, Rudisch A, Innerhofer K, Brandlmaier I, Moshen I, Bertram S. Magnetic resonance imaging findings of internal derangement in temporomandibular joints without a clinical diagnosis of temporomandibular disorders. J Oral Rehabil 2002: 29: 516–522.
Emshoff R, Rudisch A. Validity of clinical criteria for temporomandibular disorders: clinical versus magnetic resonance imaging diagnosis of temporomandibular joint internal derangement and osteoarthrosis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2001: 91: 50–55.
Fleiss JL. The measurement of interrater agreement. In: Fleiss JL, ed: Statistical Methods for Rates and Proportions 2nd Ed New York: John Wiley & Sons 1981: 212–236.
Haiter-Neto F, Hollender L, Barclay P, Maravilla KR. Disk position and the bilaminar zone of the temporomandibular joint in asymptomatic young individuals by magnetic resonance imaging. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2002: 94: 372–378.
Huddleston-Slater JJ, van selms MK, Lobbezoo F, Naeije M. The clinical assessment of TMJ sounds by means of auscultation, palpation or both. J Oral Rehabil 2002: 29: 873–878.
Katzberg RW, Westesson PL, Tallents RH, Drake CM. Anatomic disorders of the temporomandibular joint disk in asymptomatic subjects. J Oral Maxillofac Surg 1996: 54: 147–153.
List T, Dworkin SF. Comparing TMD diagnoses and clinical findings at Swedish and US TMD center using Research Diagnostic Criteria for Temporomandibular Disorders. J Orofac Pain 1996: 10: 240–253.
MANFREDINI D, BASSO D, SALMASO L, GUARDA-NARDINI L. Temporomandibular joint click sound and magnetic resonancedepicted disk position: which relationship? J Dent 2008: 36: 256–260.
Manfredini D, Chiappe G, Bosco M. Research Diagnostic Criteria for Temporomandibular Disorders (RDC/TMD) axis I diagnoses in an Italian patient population. J Oral Rehabil 2006: 33: 551–558.
Manfredini D, Segu` M, Bertacci A, Binotti G, Bosco M. Diagnosis of temporomandibular disorders according to RDC/TMD Axis I findings. A multicenter Italian study. Minerva Stomatol 2004: 53: 429–438.
Marguelles-Bonnet RE, Carpentier P, Yung JP, Defrennes D, Pharaboz C. Clinical diagnosis compared with findings of magnetic resonace imaging in 242 patients with internal derangement of the TMJ. J Orofac Pain 1995: 9: 244–253.
Matsuda S, Yoshimura Y, Lin Y. Magnetic resonance imaging assessment of the temporomandibular joint in disk displacement. Int J Oral Maxillofac Surg 1994: 23: 266–270.
Orsini MG, Kuboki T, Terada S, Matsuka Y, Yatani H, Yamashita A. Clinical predictability of temporomandibular joint disk displacement. J Dent Res 1999: 78: 650–660.
Rammelsberg P, Jager L, Pho Duc JM. Magnetic resonance imaging-based joint space measurements in temporomandibular joints with disk displacements and in controls. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2000: 90: 240–248.
Roberts C, Katzberg RW, Tallents RH, Espeland MA, Handelman SL. The clinical predictability of internal derangement of the temporomandibular joint. Oral Surg Oral Med Oral Pathol 1991: 71: 412–414.
Sato S, Nasu F, motegi K. Natural course of nonreducing disk displacement of the temporomandibular joint: changes in chewing movement and masticatory efficiency. J Oral Maxillofac Surg 2002: 60: 867–872.
Schmitter M, Kress B, Rammelsberg P. Temporomandibular joint pathosis in patients with myofascial pain: a comparative analysis of magnetic resonance imaging and a clinical examination based on a specific set of criteria. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2004: 97: 318–324.
Tasaki M, Westesson PL. Temporomandibular joint: diagnosing accuracy with sagittal and coronal MR imaging. Radiology 1993: 186: 723–729.
Tognini F, Manfredini D, Montagnani G, Bosco M. Is clinical assessment valid for the diagnosis of temporomandibular jont disk displacement? Minerva Stomatol 2004: 53: 439–448.
Truelove EL, Sommers EE, Leresche L, Dworkin SF, Von Korff M. Clinical diagnostic criteria for TMD: new classification permits multiple diagnoses. J Am Dent Assoc 1992: 123: 47–54.
Watt-Smith S, Sadler A, Baddeley H, Renton P. Comparison of arthrotomographic and magnetic resonance images of 50 temporomandibular joints with operative findings. Br J Oral Maxillofac Surg 1993: 31: 139–143.
Westesson PL, Erikson L, Kurita K. Reliability of a negative clinical temporomandibular joint examination: prevalence of disk displacement in asymptomatic temporomandibular joint. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1998: 68: 551–554.
Westesson PL, Paesani D. MR imaging of the TMJ: decreased signal from the retrodiskal tissue. Oral Surg Oral Pathol Oral Med 1993: 76: 631–635.
Westesson PL. Reliability and validity of imaging diagnosis of temporomandibular joint disorder. Adv Dent Res 1993: 7: 137–151.
Wolfe F, Smythe HA, Yanus MB, Bennet R, Bombardier C, Goldenberg G et al. The American College of Rheumatology 1990 Criteria for the Classification of Fibromyalgia: Report of the Multicenter Criteria Committee. Arthritis Rheum 1990: 33: 160–172.
Yap AJU, Dworkin SF, Chua EK, List T, Tan KBC, Tan HH. Prevalence of temporomandibular disorders subtypes, psycologic distress and psychosocial dysfunction in asian patients. J Orofac Pain 2003: 17: 21–28.
Yatani H, Sonoyama W, Kuboki T, Matsuka Y, Orsini MG, Yamashita A. The validity of clinical examination for diagnosing anterior disk displacement with reduction. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1998: 85: 647–653.
Yatani H, Suzuki K, Kuboki T, Matsuka Y, Maekawa K, Yamashita A. The validity of clinical examination for diagnosing anterior disk displacement without reduction. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1998: 85: 654–660.
