Gingival Surgery Techniques
Machine translation
Original article is written in RU language (link to read it) .
There are various surgical techniques for treating periodontal diseases. The most common operations include gingivectomy, gingivoplasty, and flap surgery. However, the search for new surgical periodontology techniques continues, which would allow for the sanitation of deep periodontal pockets, inactivation of pathogenic microorganisms, and enhancement of osteogenesis processes.
Training in the techniques for treating periodontal tissue diseases is offered in the online course Master Class in Surgical Periodontology: Techniques and Innovations.
Gingivectomy
This is a surgical intervention aimed at sanitizing the periodontal pocket, based on the incision of the pocket wall, scraping off granulations, dental deposits, and evacuation of purulent discharge. This technique is used when a patient is diagnosed with moderate or severe periodontitis, with the addition of abscess formation, if the pathological focus is limited to several adjacent teeth.
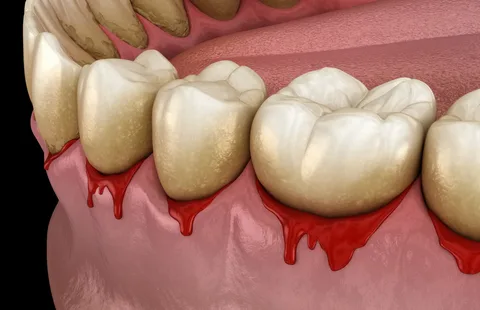
Figure 1. Symptoms of periodontal disease.
Procedure Technique
- Adequate anesthesia.
- Performing an incision. The direction of the incision is determined by the clinical picture. Mucosal incisions can be horizontal, vertical, or diagonal. The incision is made either in the projection of the central part of the periodontal pocket or around its periphery. It is essential to avoid cutting through the gingival margin; a 2-3 mm section up to the edge of the gum must be preserved. Otherwise, the edges of the wound may separate, leading to root exposure.
- The incision is made to the full depth of the pathological pocket, ensuring reliable sanitation.
- The mucous membrane and periosteum are detached along the entire length of the surgical wound.
- Curettage is performed, removing all granulations and altered tissues.
- Soft decalcified bone tissue is removed using a burr or a special bone spoon.
- The cessation of bleeding is a sign of thorough granulation removal.
- Antiseptic treatment of the surgical field.
- Some specialists recommend filling the bone pockets with bone grafts, antibiotics, or synthetic bone substitutes.
- Suturing is applied, and using special glue to bond the edges is permissible.
- In cases of copious purulent discharge, or if a vertical incision was made, such wounds are not sutured.
The main advantage of gingivectomy is the absence of gum retraction after the procedure.
Disadvantages of the gingivectomy technique:
- it is not possible to treat several pathological sites from one wound;
- proliferated epithelium is not removed;
- due to the need to preserve the gingival margin, the incision does not allow a full view of the surgical field.
Gingivectomy
Partial gingivectomy is a technique that helps preserve an extended section of the gum.
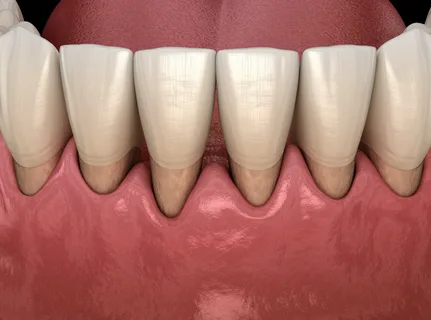
Figure 2. Root exposure.
Procedure Technique
- Adequate anesthesia.
- Making a horizontal incision, retreating 1.5-2 from the gum edge, with incisions made on both sides of the alveolar process: oral and vestibular.
- Sanitation of the pathological pocket.
- Antiseptic treatment, applying a dressing.
The main advantage of this technique is considered to be the elimination of gingival pockets.
However, this technique has its drawbacks:
- bone pockets are only partially treated, which is associated with poor visibility;
- exposes the necks of the teeth;
- under the influence of chemical and thermal irritants, the exposed roots experience severe pain, which will subsequently require additional treatment.
Diathermocoagulation
This is an electrosurgical method based on the use of high-frequency currents.
The indications for diathermocoagulation may be as follows:
- hypertrophic gingivitis;
- periodontitis, if the depth of the pockets is more than 3 mm;
- gingival fibromatosis;
- joining of abscess formation.
The work is carried out on special devices that are switched to "cutting" mode.
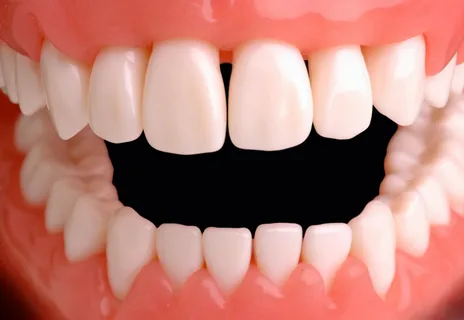
Figure 3. Moderate periodontitis.
Procedure Technique
- Thorough drying of the surgical field.
- The electrode is placed at the very base of the abscess or hypertrophied papilla, and current is applied.
- The instrument is smoothly inserted to the required depth.
- Subsequently, necrotized tissues are removed.
- Antiseptic treatment of the wound.
- Application of a non-hardening dressing with hormonal drugs, antibiotics, enzymes, and keratoplastic agents.
- After 1-2 days, the dressing is removed, and the mucosa is washed with a warm antiseptic solution.
- Wound healing occurs within two weeks.
There is a so-called bioactive technique, where one of the electrodes is placed on the outside of the pocket, while the second one is inserted directly into the pocket. After the device is turned on, the instrument is smoothly advanced horizontally into the pocket.
Advantages of diathermocoagulation:
- electric current has good bactericidal properties;
- due to the absence of bleeding, an excellent view of the surgical field is maintained.
The main disadvantage of this technique is the high risk of damaging intact mucosa, as well as burns to the vessels and nerves of the pulp.
Cryodestruction
This manipulation involves the removal of formations and pathologically altered tissues, which is carried out under the influence of low temperatures that contribute to cell death. The following can be used as freezing agents: oxygen, freon, liquid nitrogen, carbon dioxide.
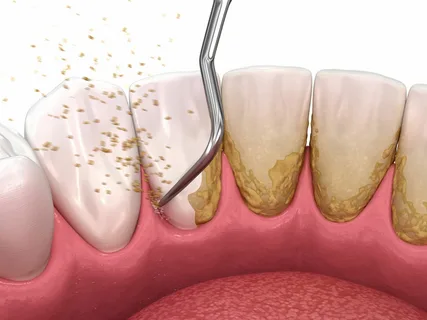
Figure 4. Removal of dental deposits.
Indications for cryodestruction:
- hypertrophic gingivitis;
- forms of periodontitis, with a diagnosed depth of pathological pockets equal to 5–7 mm.
The significant thinning of the periodontal pocket wall is a contraindication for cryodestruction.
Technique of procedure
- Anesthesia.
- Preoperative preparation of the surgical field.
- The applicator is immersed in the coolant.
- The cryoapplicator is smoothly inserted to the full depth of the pocket.
- The duration of cryo-exposure is no more than 10 seconds.
- Several periodontal pockets are treated simultaneously, but no more than five in one session.
- No dressing is required after cryodestruction. Antiseptic treatment of the surgical field is sufficient.
- On the third day, proteolytic enzymes are placed in the treated pockets, introduced on turundas.
- After 3-4 days, the pocket is completely freed from necrotic masses, and regeneration processes begin.
- From the fifth day, dressings with antibiotics and keratoplastics are used.
- Completion of regeneration processes is observed after 4-6 days.
Laser Coagulation
In gingival surgery, a laser scalpel is used, which operates based on a carbon dioxide laser. A carbon dioxide laser is a gas laser with the highest efficiency ratio. The active medium of the carbon dioxide laser consists of a mixture of helium (82%), nitrogen (13.5%), and carbon dioxide (4.5%).
The principle of the laser's operation as a coagulator or cutting tool is based on the conversion of electromagnetic energy into heat. The carbon dioxide laser penetrates the tissue to a depth of 0.1 mm. The absorbed light is converted into heat, the local temperature of the tissues reaches 300 °C, resulting in the evaporation of the tissue. The use of this type of laser is accompanied by the formation of a zone of thermal necrosis, which is minimal in size.
Modern models of carbon dioxide lasers used in gingival surgery are compact, equipped with flexible steel waveguide shafts, which make it easy to reach the most inaccessible areas of the oral cavity.
The advantages of using a laser are as follows:
- the wound remains sterile;
- no bleeding;
- no need for sutures;
- minimal pain during the operation;
- tissue healing occurs without scars.
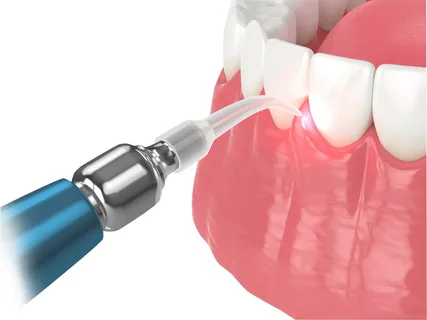
Figure 5. The use of laser in dentistry.
Indications for the use of a carbon dioxide laser:
- gingivectomy,
- gingivoplasty,
- sterilization of the periodontal pocket.
Technique of Procedure
- Anesthesia.
- Thorough removal of dental deposits.
- Using a laser beam, gingivectomy is performed on both sides of the alveolar process: oral and vestibular, to a depth of the periodontal pocket of 2-3 mm.
- Curettage is performed, root smoothing is carried out.
- The epithelial lining of the periodontal pocket is denatured under the influence of the laser beam over its entire inner surface. A carbonized wound surface is formed.
- The surface of the pocket is periodically treated with wipes soaked in saline or antiseptics.
- Epithelialization occurs within up to two weeks.
Complete information about surgical and non-surgical methods of periodontal treatment is collected in the online course Advanced Periodontal Treatment. Surgical and Non-Surgical Approaches.