Curettage as a method of gingival surgery
Periodontal disease remains the most challenging problem for modern dentistry today. The methods of surgical treatment of periodontal diseases currently presented are very diverse. Curettage and flap operations are of key importance in the prevention of periodontal diseases.
Detailed protocols for the surgical treatment of periodontal diseases in the online course Surgical Periodontology .
Experts are still trying to develop effective surgical protocols that will revolutionize the sanitation of periodontal pockets, will promote persistent inhibition of pathogenic microorganisms and activate osteogenesis, and will improve the structure and functioning of periodontal tissues.
Curettage
Curettage is a gentle surgical procedure that is widely used for periodontal diseases. This procedure is also one of the components of other methods of surgical periodontology: gingivotomy, gingivectomy and flap operations.
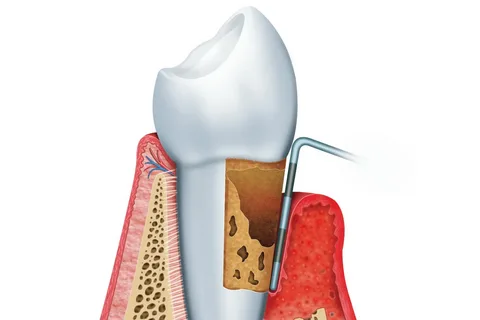
Figure 1. Periodontal disease.
The main purpose of curettage is to clean the surface of the teeth from dental plaque located under the gum, remove granulations, and scrape the epithelium from the gingival edge of the pocket.
The following indications for curettage can be distinguished:
The depth of the periodontal pocket cannot exceed 4 mm.
It is used for diagnosed periodontitis of mild severity, rarely for moderate severity.
This method of gingival surgery has its own contraindications:
Attachment of acute inflammation in the area of proposed manipulation, purulent exudation, abscess formation.
Excessive thinning of the gingival wall of the periodontal pocket.
Definition of bone pockets.
Methodology
The technique of curettage involves the following steps:
Anesthesia, infiltration or conduction anesthesia, carpule anesthetic can be used.
The surgical area within several adjacent teeth is treated with antiseptic solutions (furacillin, chlorhexidine, hydrogen peroxide); it is advisable to use weak solutions of these drugs, since solutions in high concentrations will slow down postoperative regeneration. To prevent infection of the wound surface with oral fluid, the teeth in the surgical area are wrapped with sterile pads.
Subgingival hard deposits, as well as pathologically modified cement, are removed using sharply sharpened instruments: excavators, hooks of various shapes and sizes (mechanical method). It is important to carry out processing in strict sequence so as not to miss anything. We start with the vestibular surface, then we clean the proximal ones, and finally the oral surface. During the curettage process, movements are directed from the depths of the pocket towards the crown; they are carried out in the vertical plane, horizontal, and also diagonally. The use of movements of various directions during curettage helps to increase the efficiency of cleansing the root from modified tissues and dental deposits. To prevent periodontal injury, the tooth is securely fixed with the thumb and index finger of the left hand.
The root cement is treated with finishers and polishers. You can use pneumatic tools powered by compressed air; they are capable of removing a layer of 5–7 microns of hardened dental plaque.
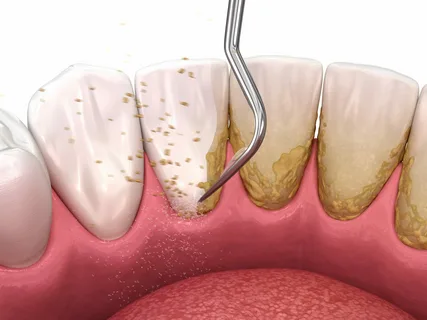
Figure 2. Removal of dental plaque.
The use of peripolers (curettes) fixed in the contra-angle handpiece ensures smoothing of the root surface. To clean the furcation area and root bends, periotomes are used - these are devices equipped with many notches.
Scaling is the process of removing tartar using ultrasound.
How is tartar formed?
Dental plaque is formed as a result of mineralization of plaque contaminated with microorganisms, which occurs under the influence of saliva. Mineralization of subgingival dental plaque occurs with the participation of gingival fluid. Tartar has a rough, bumpy surface, which promotes the further attachment of new colonies of microorganisms and their gradual mineralization.
Attachment of tartar to the surface of the tooth is carried out due to the formation of a kind of crust or shell on the root, penetration of microcracks in the cement, filling of resorbed foci located in dentin or cement.
Hard dental deposits in the furcation area and in the root grooves are anatomically inaccessible. Tartar located above the gum is light in color from creamy white to dark shades of yellow and is easier to remove. Subgingival deposits are characterized by a greater density of structure and are darker in color, often brown.
Tartar removal
To clear hard-to-reach areas from subgingival stone, thin scaler attachments and sharp aggressive instruments are used; in the settings, higher power and minimal vibration amplitude are used. In the process of removing deposits, minimal pressure should be applied to the tooth, but to chip away stones, significant pressure is required (minimum amplitude of vibration).
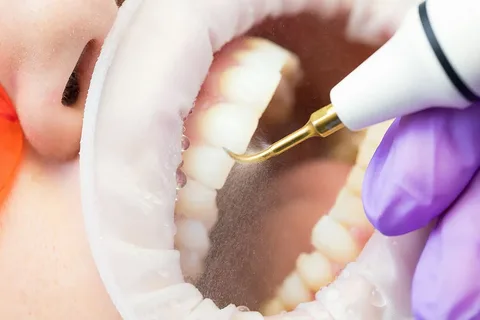
Figure 3. Ultrasonic tartar removal.
If the surface of the cement is riddled with small cracks into which dental plaque penetrates, subgingival stones are removed along with small fragments of cement. The cement preserved between microcracks forms retention points for recolonization by microorganisms and promotes the formation of new stone.
Hence the importance of making the cement smooth, but it is important to remember the principle of gentle excision of hard tooth tissue. It is better to give preference to less aggressive thin nozzles:
diamond for root leveling and cement remodeling,
carbon fiber for excision of normal or low mineralized plaque.
To visually determine the presence of plaque, a special detection solution is used. Metabolic products of pathological microflora are found only in the surface layer of cement. In the process of ultrasonic treatment, most of the microorganisms of the periodontal pocket die; this result cannot be achieved by mechanically cleaning the root surface from stone, but complete destruction of the flora is not observed with any method. In this regard, during curettage, the pocket must be rinsed with antiseptic drugs.
When performing several scaling procedures with a minimum interval between visits for 1-2 months, you can achieve significant suppression of the growth of colonies of microorganisms. Consolidation of bone structures occurs over six months against the background of subgingival irrigation and regular cleaning of the back of the tongue using antiseptics for two weeks.
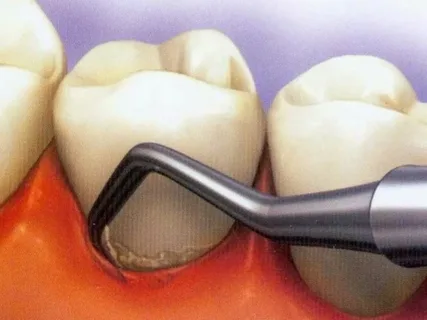
Figure 4. Subgingival dental plaque.
A combined approach - the simultaneous use of hand instruments and ultrasound gives the most effective result in the fight against hard dental plaque. Maintenance therapy is indicated every three months. It should not be carried out invasively relative to the root surface; it is enough to clean the surface of soft plaque. To do this, you can use composite carbon tips.
Excision of granulations and deepithelialization
The pocket cavity is washed under pressure with an antiseptic solution, this helps to get rid of the smallest particles. The remains of unremoved fragments of subgingival deposits are dissolved chemically: 20% lactic and 5% citric acids. To facilitate the attachment of fibroblasts to the cement after mechanical cleansing of the tooth root and treatment with acid, fibrinonictin is applied to the surface. Excess is removed, the treated area must be isolated from oral fluid for half an hour.
Then, using a sharp excavator, the granulations are scraped out of the pocket. The alveolar bone is subjected to careful, gentle treatment. The stability factor of a periodontal pocket is the epithelium that has grown into it; a prerequisite for the effectiveness of curettage is de-epithelialization of the pocket - curettage of the germinated epithelium.
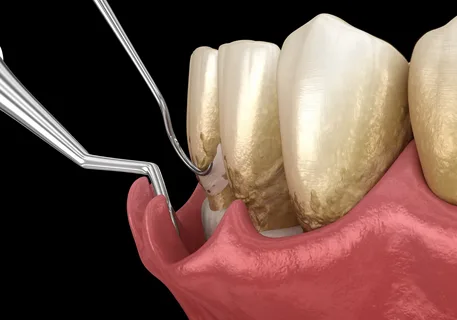
Figure 5. Performing curettage.
The cut epithelium exposes the wound surface, which subsequently adheres to the cement. It is important to completely excise the strips of epithelium; remaining fragments will cause relapse.
A sharp instrument is inserted into the bottom of the pocket. The gum is pressed against the root with a finger. With a smooth movement of the instrument, granulations and epithelium are cut off, the direction of movement is towards the crown. Next, the pocket is filled with heated saline solution. The formed blood clot is subsequently converted into connective tissue, which will tighten the surface of the pocket. Connective tissue fibers will grow into the layer of newly formed cement. Epithelization and restoration of the gap will occur in the next 7–10 days, collagen fibers will form by the end of the third week.
More up-to-date information on the surgical treatment of periodontal diseases in the online course Surgical periodontology: preparation for prosthetics .
