Guided Surgery – Digital Workflow
Machine translation
Original article is written in PT language (link to read it) .
The use of the first osseointegrated implants to replace missing dental elements, nearly 50 years ago, represented a huge evolution in dental rehabilitation techniques. Over the years, many solutions have been proposed with the aim of improving the clinical performance of dental implants. The shape of the implant has evolved with the introduction not only of cylindrical structures, more efficient spiral designs, and better implant-prosthesis connections. Many surface treatments have also been suggested to modify the nanostructure of titanium, improving the processes of osseointegration and bone healing. The scientific literature agrees that implant-supported rehabilitations have a five-year survival rate of approximately 95% and over 89% after 10 years. However, the current trend in implant surgery is to further improve these clinical procedures, reducing the total rehabilitation time while using less invasive surgical techniques. Guided implant protocols could help physicians simplify their procedures, from the diagnostic phase to the execution of final prosthetic restorations. The first and probably the most important stage for the development of these new clinical procedures was the introduction and dissemination of three-dimensional (3D) imaging techniques and computerized technology. These allowed for the improvement of traditional pre-surgical planning, in which radiographic assessments were used, often through periapical and panoramic radiographs, study models, and direct inspection of the alveolar ridges. The evaluation of 3D data, extracted from computed tomography, but also more recently from intraoral scanners, along with modern implant planning software, allows for careful simulation of the surgical and prosthetic phases.

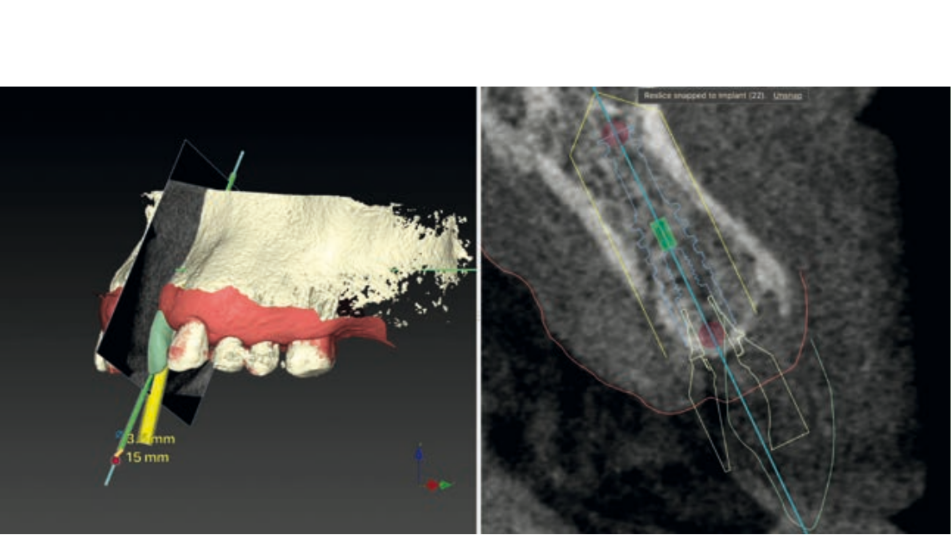
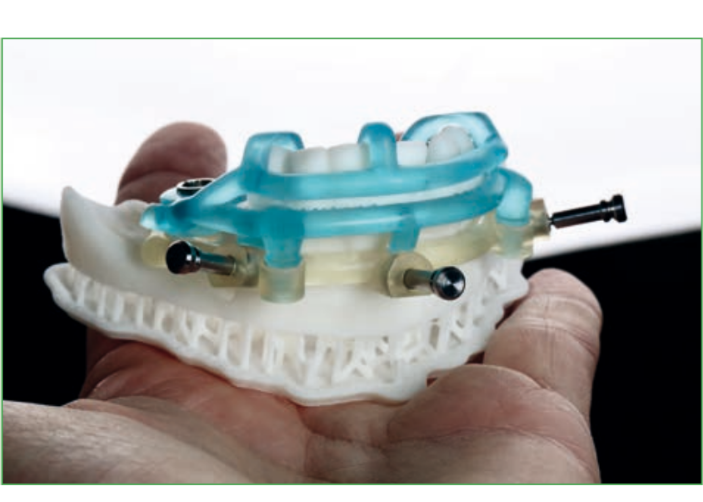
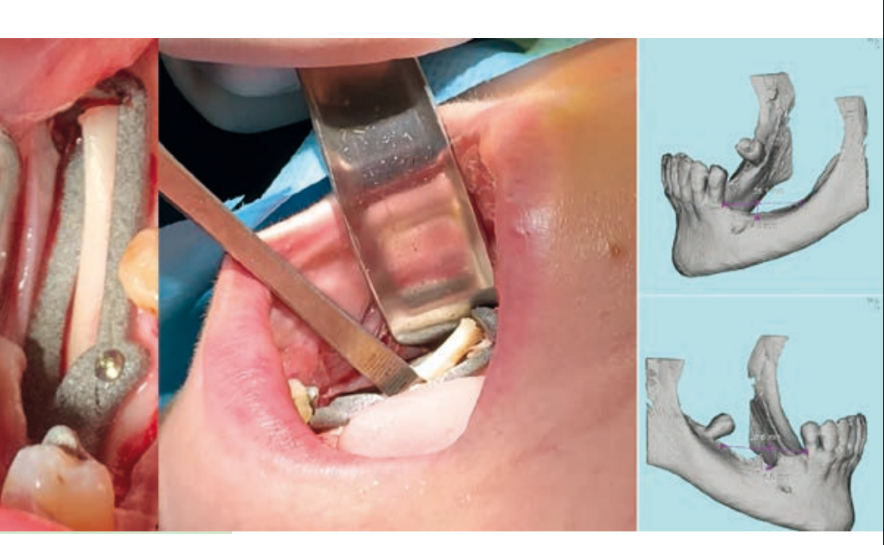
The locations of the implants can be decided before the surgery according to the volume and quality of bone, the location of anatomical structures (nerves, vessels, or other anatomical structures), prosthetic and aesthetic evaluations. Accurate and individual measurements of the width and height of the bone at planned implant sites, as well as distances and angles between implants from one side to the other of an arch, can be predetermined without the distortions present in the two-dimensional format. The implants and abutments can then be planned "virtually," guided by the knowledge of the position of the planned restoration. It also allows for the predetermination of the insertion path of the prosthesis, the space of the components, and pre-surgical abutment choices, as well as the pre-surgical production of individual abutments. Accurate virtual surgery planning can sometimes avoid bone augmentation procedures that are associated with prolonged treatment times and sometimes, unfortunately, also with serious clinical complications. Furthermore, careful three-dimensional positioning of the implants allows for the best clinical outcomes, especially regarding aesthetic aspects.
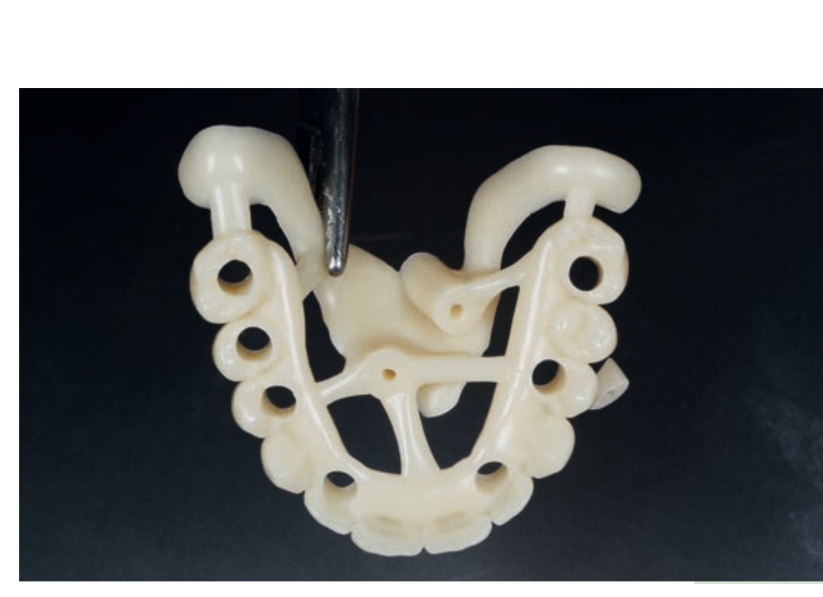
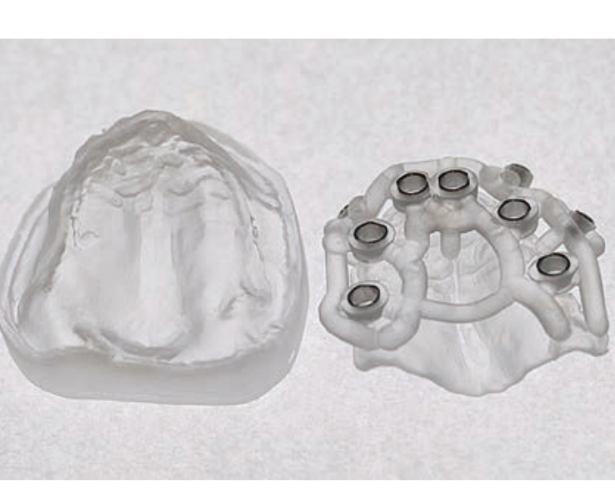
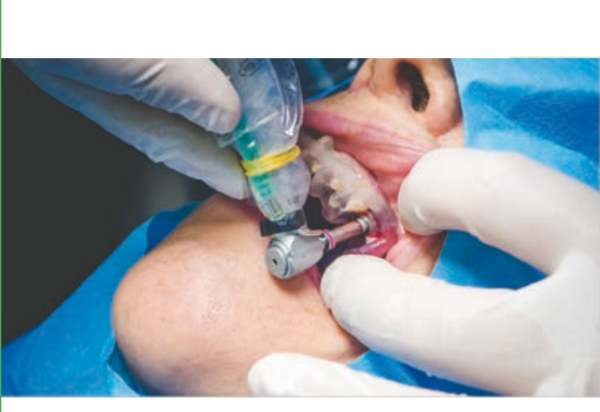
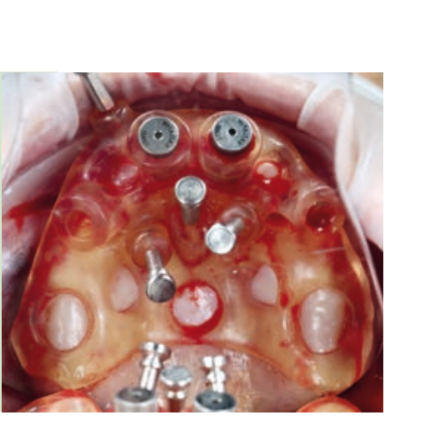
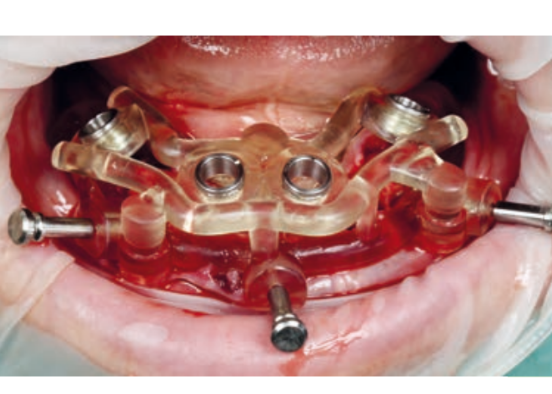
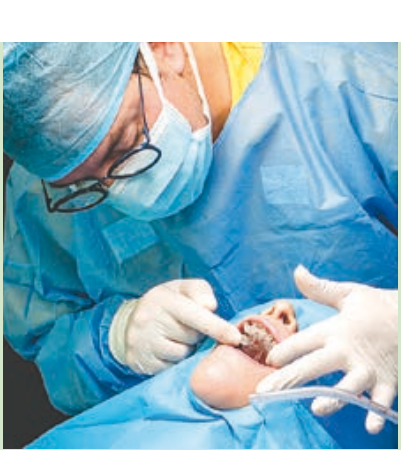
Guided implant surgery allows the transfer of the planned rehabilitation project directly to the surgical field. The clinician can choose between several guided methods; initially, surgical guides can be divided into "static" and "dynamic." The latter are represented by guided navigation methods where a computer-guided navigation system assists the clinician in real-time during the positioning of the implant through visual imaging tools on a monitor. These methods, although very interesting from a future perspective, are not currently particularly widespread. The "static" methods include, instead, the use of surgical guides that can be produced by conventional procedures, modifying a radiographic scanning prosthesis or through Computer-Aided Design/Computer-Aided Manufacturing (CAD/CAM) technologies (milling/stereolithography or 3D printing).
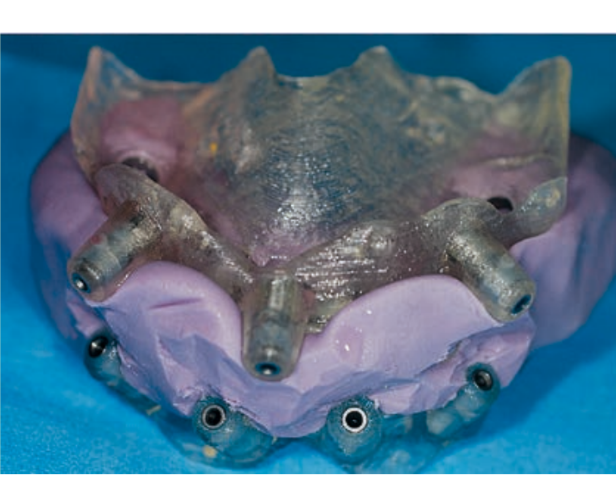
Surgical guides can be supported on teeth, bones, or mucosas, with or without stabilization pins. Some guided systems use different guides with different ring sizes for each patient, while others use only guides without rings. An additional differentiation is given by the method of implant screwing after the preparation of the implant site: some systems provide for the fully guided insertion of the implant through the same drilling model; other methods may require the manual insertion of the implant after the removal of the surgical splint.
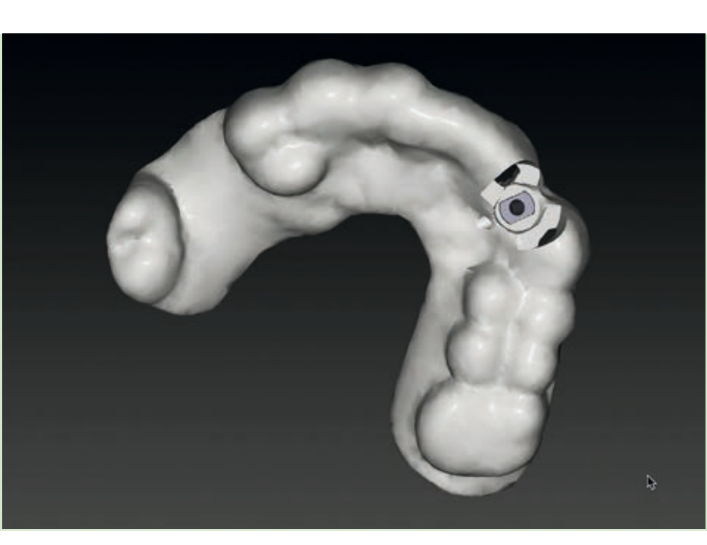

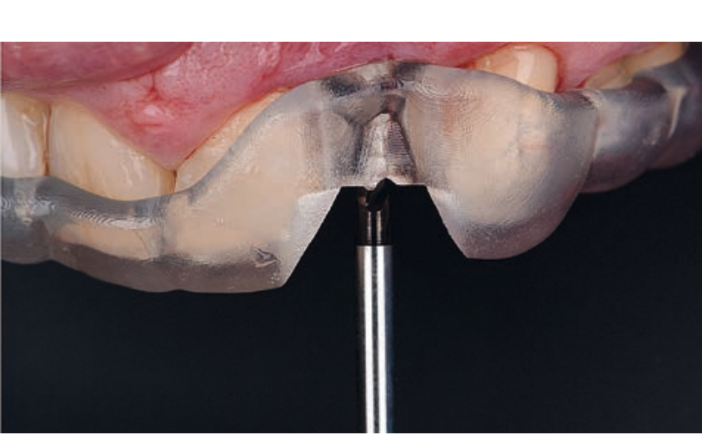
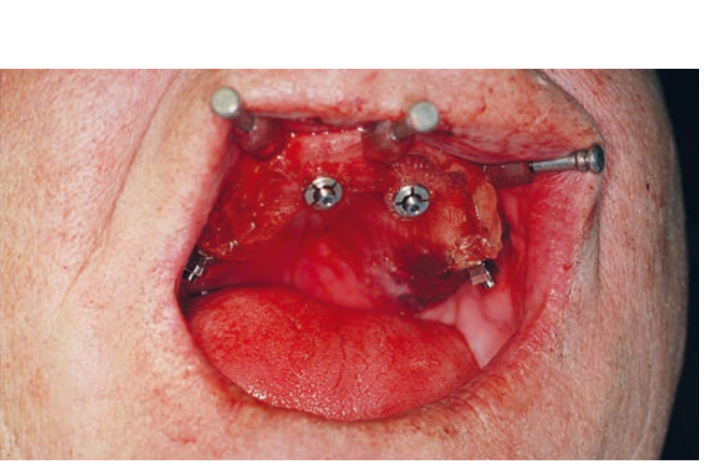
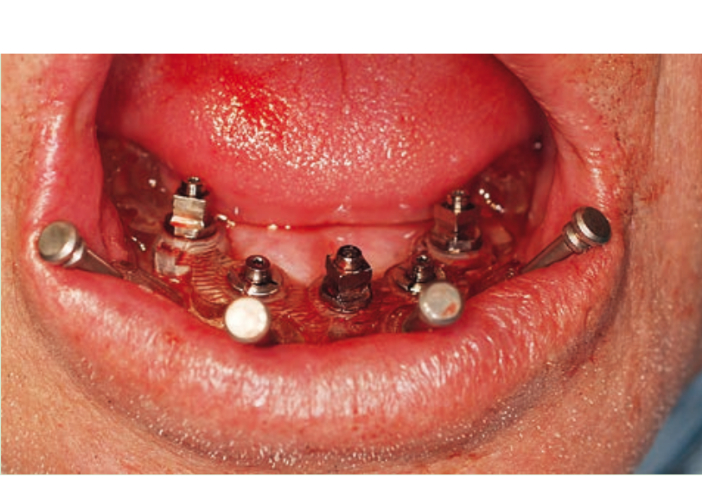
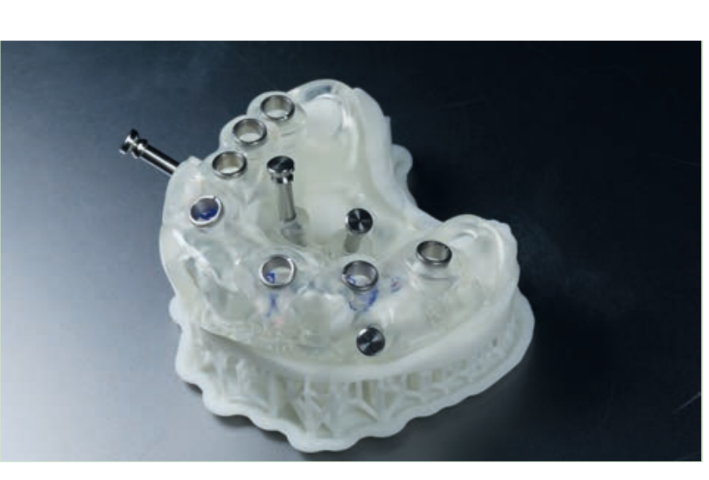
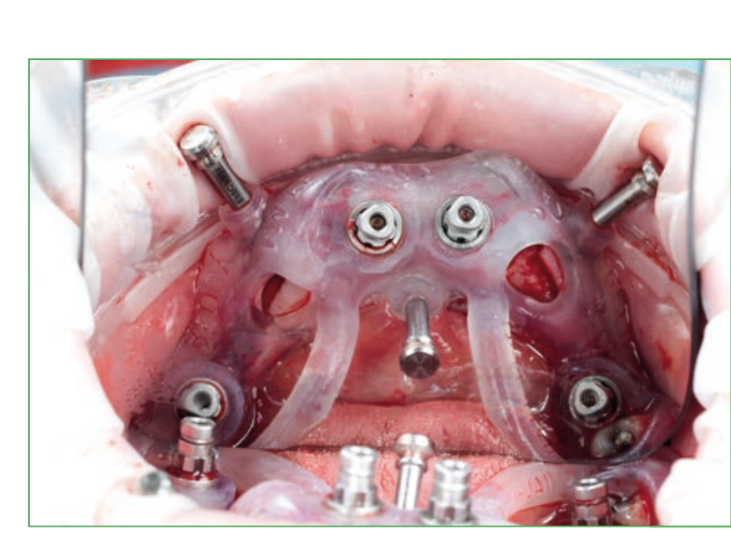
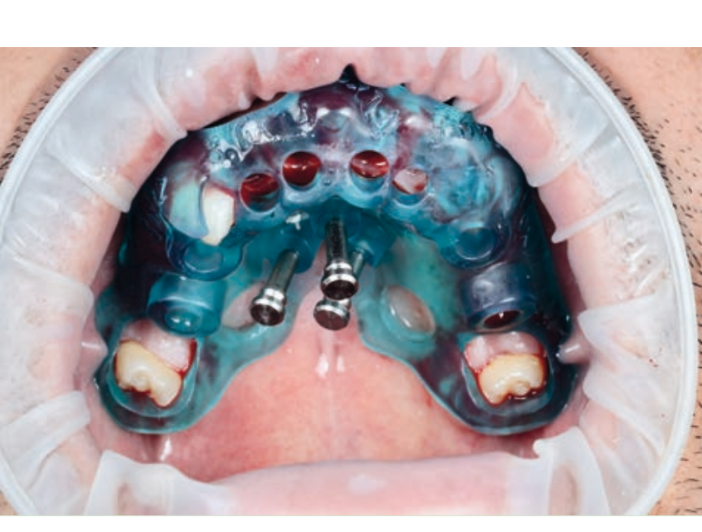
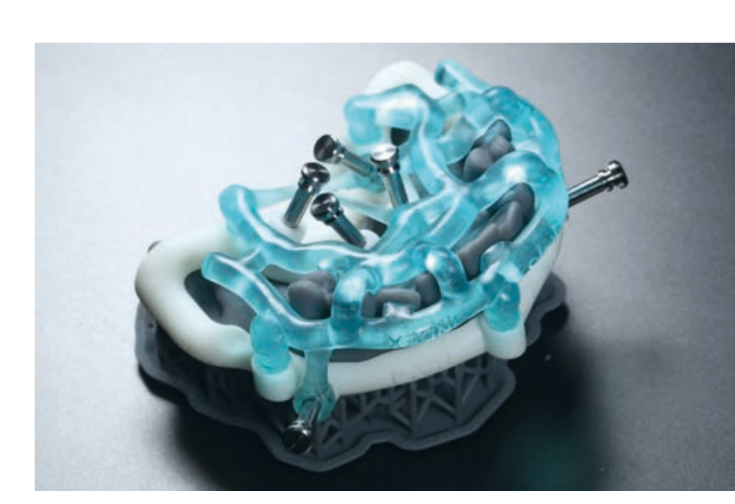

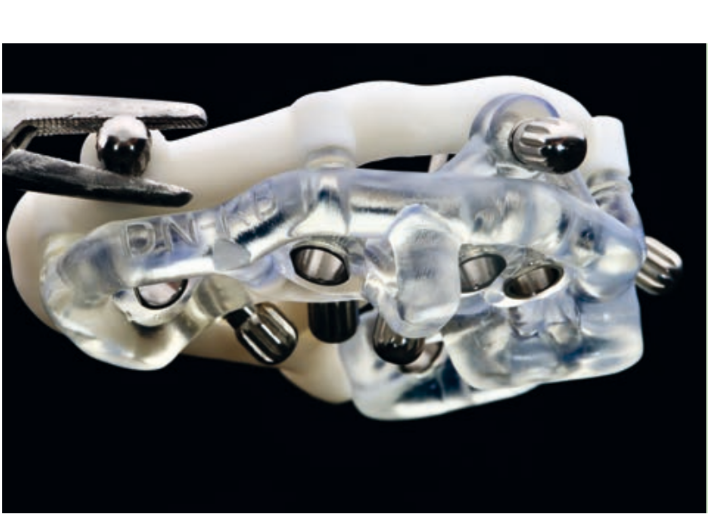
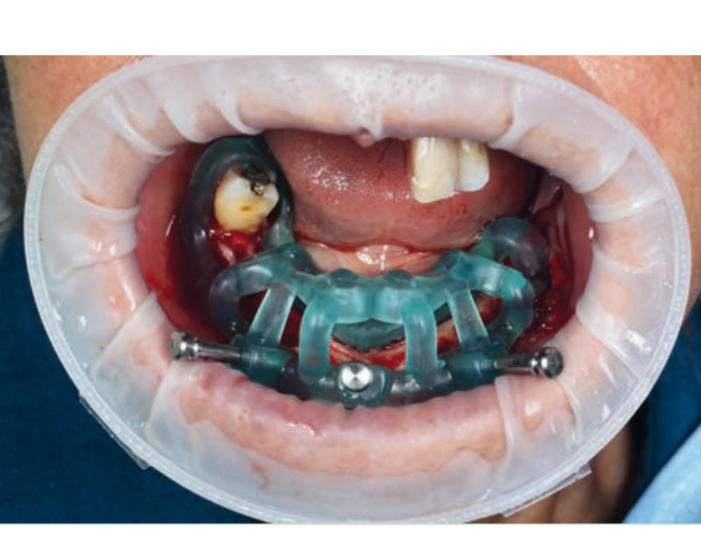
Guided implant insertion often allows for minimally invasive surgeries without the need to elevate a surgical flap. Another advantage of guided techniques is having, at the time of surgery, a prefabricated fixed prosthesis, based on the planned position of the implants, capable of connecting newly inserted implants and easily achieving a functional and aesthetic immediate load.

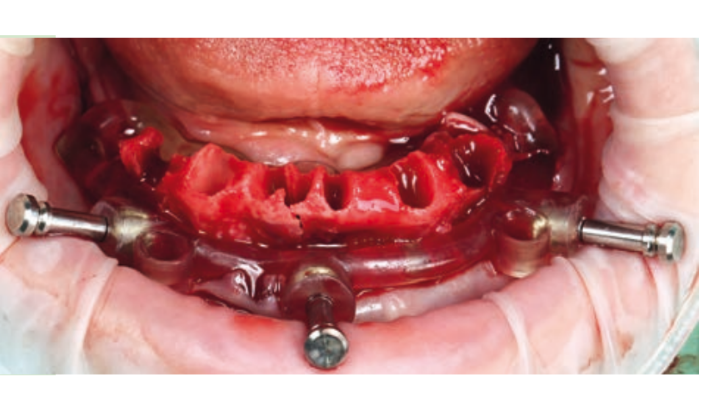
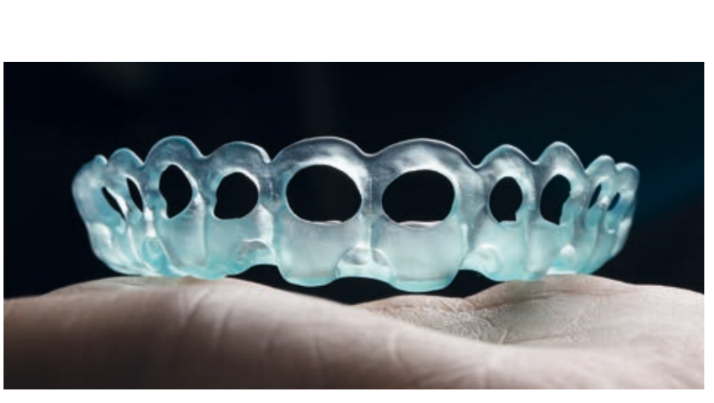

However, even for guided implant surgery, there are disadvantages that must be clearly evaluated. First of all, like all new methods, this type of surgery requires a learning period for the dentist, the technician, and generally for the entire dental team. The time required for guided pre-surgical planning of the implant is definitely greater compared to traditional protocols. Economic aspects must also be evaluated regarding training, instrumentation, and the fabrication of surgical guides. Any error in acquiring the 3D image or in the intraoral scanning leads to a distortion in the fabrication of the guide, which will result in an error in the placement of the implant and the provisional prosthesis.
With the development of guides for implant placement, many other guides have emerged, such as guides for gingivectomy and crown lengthening, guides for bone reduction, guides for the removal of bone or gingival grafts, or guides for the placement of the provisional prosthesis.
Although the average deviation of guided surgery is around 3.5 degrees, it is always superior to a freehand surgery, concluding that guided surgery is a promising, minimally invasive technique that improves the final outcome of the implant position and the prosthetic rehabilitation.