Osteopathy and Cranial Dysfunction
Machine translation
Original article is written in RU language (link to read it) .
Temporomandibular joint dysfunction is caused by a complex of structural, occlusal, and muscular disorders, against the background of various humoral and psychogenic factors. This pathology is rarely associated with inflammatory diseases.
Combined treatment of TMJ dysfunction by a dentist and osteopath in the webinar The Role of Osteopathy in Modern Dentistry.
There are two main causative factors leading to the pathology of the musculoskeletal complex:
- occlusal-articular;
- psychogenic.
Occlusal Disorders
Interocclusal contacts and the resulting tension in the periodontal tissues during the chewing process through the central nervous system "reprogram" the function of the TMJ and muscles, drawing all the organs of the maxillofacial area into the pathological chain. The formation of occlusal disorders is caused by irrational prosthetics or errors in orthopedic treatment, as well as therapeutic treatment of even a single tooth affected by caries, if its natural anatomical shape and size of the crown were not restored during the procedure.
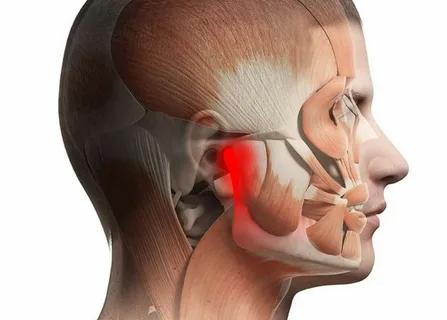
Figure 1. TMJ Dysfunction.
It is important to note the disorders of occlusion and the orthodontic treatment carried out against this background, which can lead to irreversible damage to the functioning of the temporomandibular joint, as the adaptive capabilities of the body may not cope with such a significant restructuring in all patients, which provokes the formation of dysfunction.
Structural Disorders
This group of disorders includes changes in the spatial relationships of the components of the TMJ: the articular disc, the retrodiscal area, the capsular-ligamentous apparatus, components of the condyle-muscular system.
Muscle Disorders
Caused by a disruption in the coordination of the functioning of the masticatory muscles, mechanical overload of muscle fibers, tonic spasms. A significant role in the pathogenesis of muscle disorders is played by the unilateral nature of chewing, bruxism, and the professional activities of patients whose work involves increased vocal load, including musicians. Scientific research has established that joint function pathology is associated with disturbances in the neuromuscular mechanism that controls and regulates all joint movements.
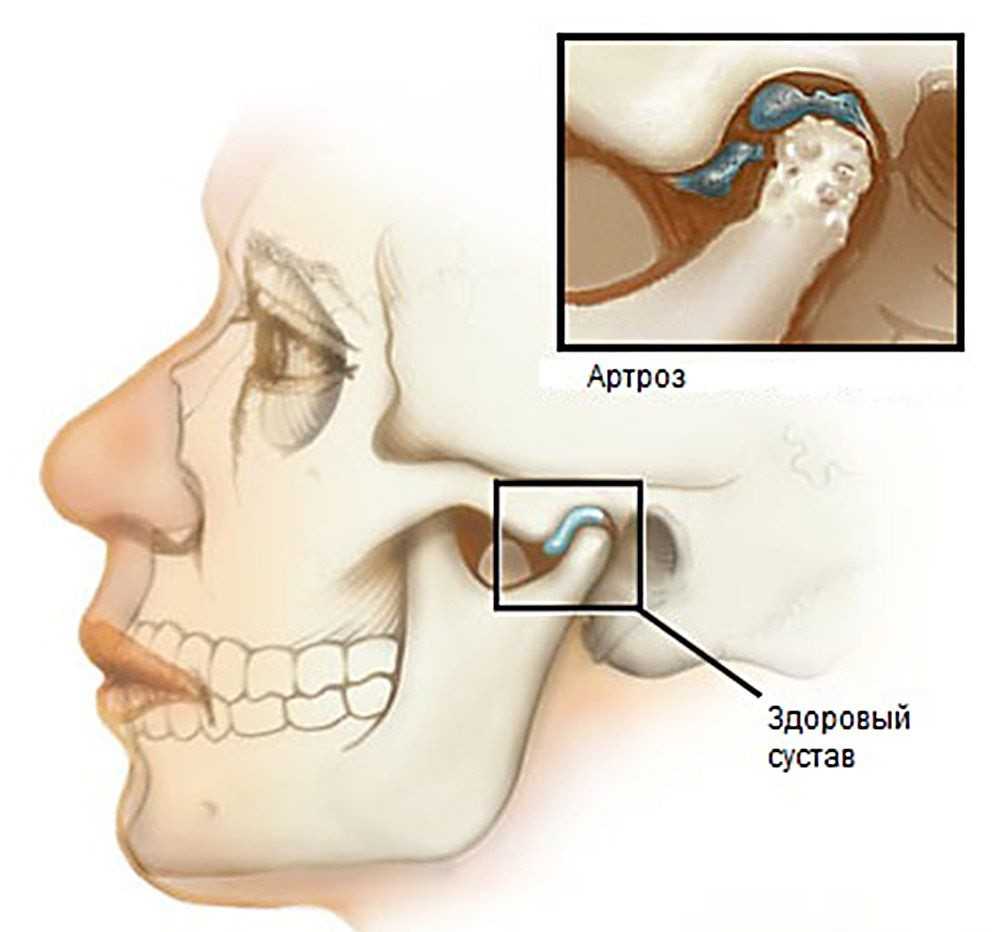
Figure 2. Structural disorders in the joint.
Psychogenic Factors
They are important etiological prerequisites for the appearance of TMJD dysfunctions, their role is as high as the influence of occlusal and structural disorders, which is explained by their close interconnection and mutual influence. Pathological articulation and irrational psychological response to a stressful situation stimulate uncoordinated contractions of different groups of masticatory muscles or their excessive strain.
Neurological Disorders
Somatic disorders of neurological origin can manifest clinically with symptoms of TMJD dysfunction, and they are most often caused by diseases of various body systems (endocrine, musculoskeletal, immune).
Traumatic Disorders
Chronic and acute traumas are a common cause of TMJD dysfunctions. In this context, macrotraumas can be identified:
- jaw fracture,
- blow,
- injuries that are not directly related to the lower jaw.
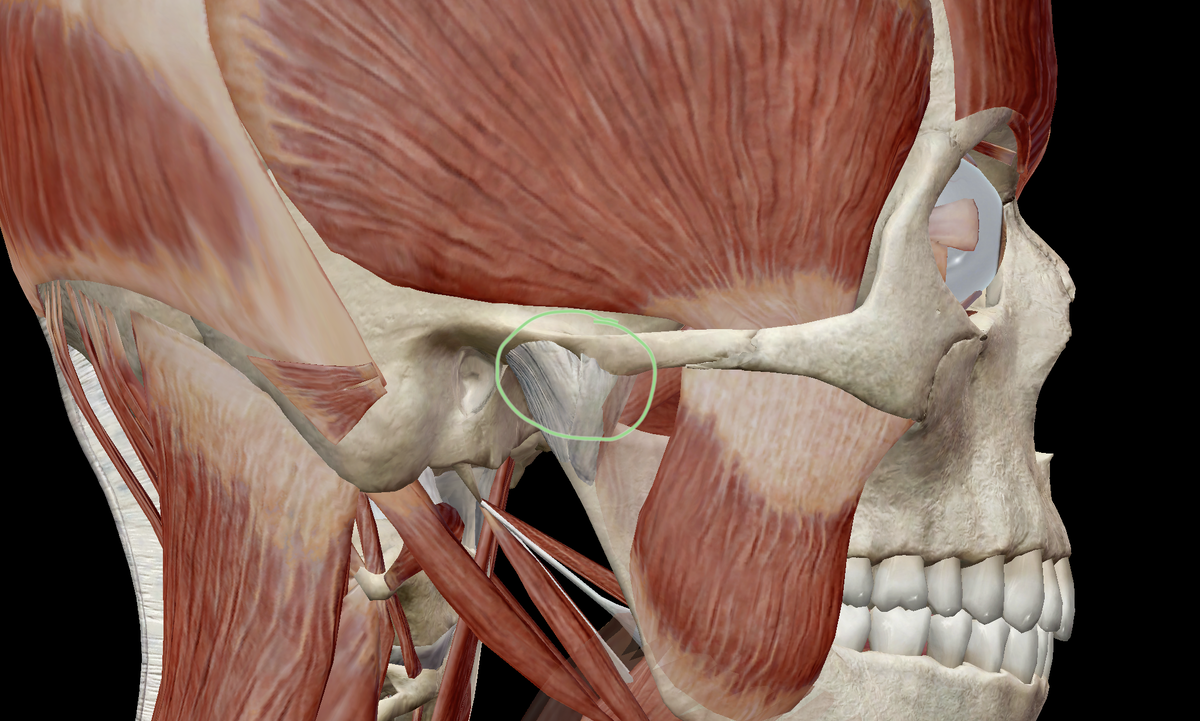
Figure 3. Chewing muscles.
Microtraumas:
- bruxism,
- premature contact on restorations, artificial crowns, bridge prostheses.
Anatomical Predisposition
Anatomical predisposition plays a special role in the formation of TMJD dysfunction.
Diseases of internal organs from various systems: cardiovascular, metabolic disorders in a stressful situation can significantly complicate the diagnosis of TMJD disorders and complicate their treatment. TMJD dysfunction, as a manifestation of systemic human diseases, involves the skeletal musculature of the head and neck in the pathological process.
If the initial pathological factor is caused by interocclusal disturbances and pathology of muscle fibers, then dysfunction first forms, and then signs of aseptic inflammation and destruction of joint tissues join, as a result of the change in the position of the joint elements.
If the primary pathological factor is a general disease (metabolic disorders, infectious processes) or traumatic injuries, then combined lesions are typical, in which symptoms of arthritis, arthrosis, or ankylosis are clearly traced.
In the etiology of TMJ dysfunction, the following groups of factors are usually distinguished: predisposing and sustaining.
Predisposing factors include:
- occlusal disorders,
- lesions of the masticatory muscles,
- morphofunctional changes in the musculoskeletal apparatus.
Sustaining factors include:
- psychovegetative syndrome,
- secondary disorders in the masticatory muscles and temporomandibular joint,
- hypocalcemia.
Examination of a patient at an osteopath's appointment
The basis of the diagnosis is the collection of the patient's main complaints at the time of the visit to the osteopath. This significantly facilitates the examination process. If the patient has specific complaints that are topographically related to the dental-jaw apparatus and the maxillofacial area, it is necessary to assume the presence of TMJ dysfunction and proceed to the subsequent examination protocol.

Figure 4. Patient examination at an osteopath's appointment.
To facilitate the task for osteopathic physicians in conducting differential diagnosis, the following tactic is recommended: the complaints presented by the patient when suspecting TMJ dysfunction are usually divided into groups.
The first group includes a specific symptom complex, which consists of complaints directly related to the TMJ, masticatory muscles, and teeth:
- noise occurring inside the joint when the lower jaw moves (crepitation, clicking, crunching);
- disruption of the trajectory and/or amplitude of movements of the lower jaw during the act of opening or closing the mouth (normally, this trajectory corresponds to a vertical straight line), lack of symmetry when opening the mouth, blocking of jaw movements;
- interocclusal discomfort;
- pain or feeling of tension in trigger points;
- increased sensitivity of tooth tissues to temperature changes;
- appearance of facial asymmetry due to hypertrophy of the temporal or more often masticatory muscle;
- occurrence of oral mucosa paresthesias (feeling of burning, dryness);
- painful sensations when chewing or biting hard food, attempting to open the mouth wide;
- voluntary or involuntary strong clenching of teeth, patient often wakes up with clenched teeth;
- increased fatigue of the masticatory muscles;
- increased wear of teeth.
The complaints listed above are a common reason for a patient's initial visit to an osteopath.
A nonspecific symptom complex, which relates to the clinical picture characterizing symptoms directly related to the temporomandibular joint, but extending beyond the masticatory apparatus:
- ear pain, sensation of noise and ringing, hearing deterioration, stuffiness, rarely the patient loses hearing;
- vision disturbances, painful sensations in the eyes, photophobia;
- limited mobility and pain in the shoulder girdle, cervical spine;
- headaches (typical localization is the occipital, forehead, temporal area), the pain is irradiating in nature;
- burning sensation in the nose, throat irritation;
- frequent dizziness;
- states of stress, depression, loss of sleep;
- decreased work capacity, increased fatigue.
Figure 5. Diagnosis of mouth opening.
These symptoms can vary in combination among different patients. Often, a single symptom is encountered, for example, limited mouth opening, or a zigzag trajectory of jaw movement when opening the mouth, or clicks are detected during the movement of the lower jaw. It is important to pay attention during the patient's examination to the appearance of early signs of pathology: sound phenomena during opening and/or closing of the mouth, periodic moderate-intensity pain in the joint area, increased fatigue of the masticatory muscles. These symptoms do not cause discomfort to patients, therefore, it is unlikely that they will seek help with them.
During a careful interview and collection of anamnesis, as well as conducting a clinical examination, if the mentioned symptoms are detected, the doctor must inform the patient, explain the importance of consulting a gnathologist or orthopedic dentist. The most favorable prognosis for treatment is observed at the early stages of pathology. In the case of advanced combined forms (ankylosis or osteoarthritis), conservative methods are not able to normalize the functioning of the TMJ.
The significance of osteopathy in clinical dental practice in the webinar The relationship between dentistry and osteopathy: the impact of osteopathic dysfunctions on dental status.
