General Characteristics of Cervical Resorption
Machine translation
Original article is written in RU language (link to read it) .
Cervical resorption is a pathological process accompanied by damage to the root tissues in the cervical area of the tooth, the development of which is due to an increase in the activity of the patient's cluster cells. This process is asymptomatic in most cases and is accidentally detected by a dentist during an examination. Treatment of cervical resorption, which occupies an extensive area of the tooth root, requires a comprehensive approach involving doctors of various specialties.
The histopathogenesis of external cervical resorption is discussed in the webinar Differential Diagnosis of Cervical Resorption.
Classification and Etiology
Diseases of tooth tissues are a common problem in adult and pediatric therapeutic dentistry today.
All diseases of tooth tissues are traditionally divided into two large groups: carious and non-carious. In turn, non-carious lesions are classified as occurring before or after tooth eruption. Trauma to the tooth is separately placed in the classification. However, in addition to the above types of tooth tissue pathology, there is another rarely encountered, not fully studied, and unpredictable in terms of prevention – resorption.
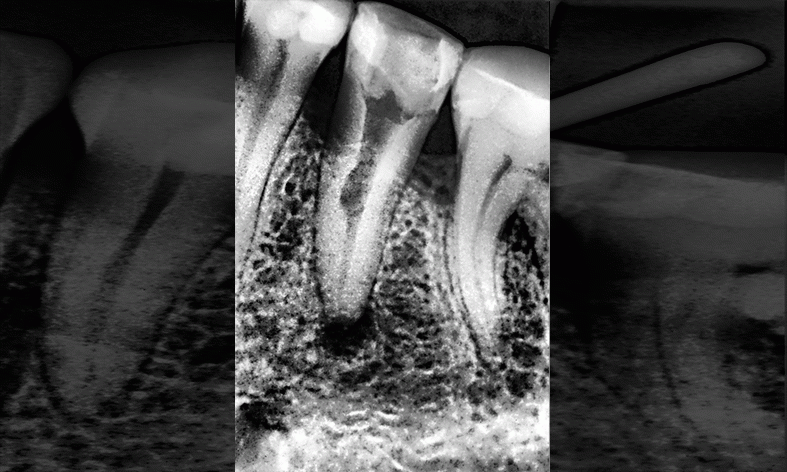
Figure 1. Example of cervical resorption.
Resorption can be observed in both vital and previously depulped teeth, clinically it is accompanied by the lysis of tooth tissues, and is caused by the active activity of the patient's clastic cells. Often, the dentist is unable to determine the cause of the development of this condition. The most popular principle of resorption classification is by its localization.
The most common types of resorption are external and internal root resorption. Cervical resorption (or invasive, external-internal) is extremely rare. It represents damage to the root tissues predominantly in the cervical area of the tooth, developing as a result of inflammatory processes against the background of activation of clastic cells on the surface of the root already involved in the pathological process.
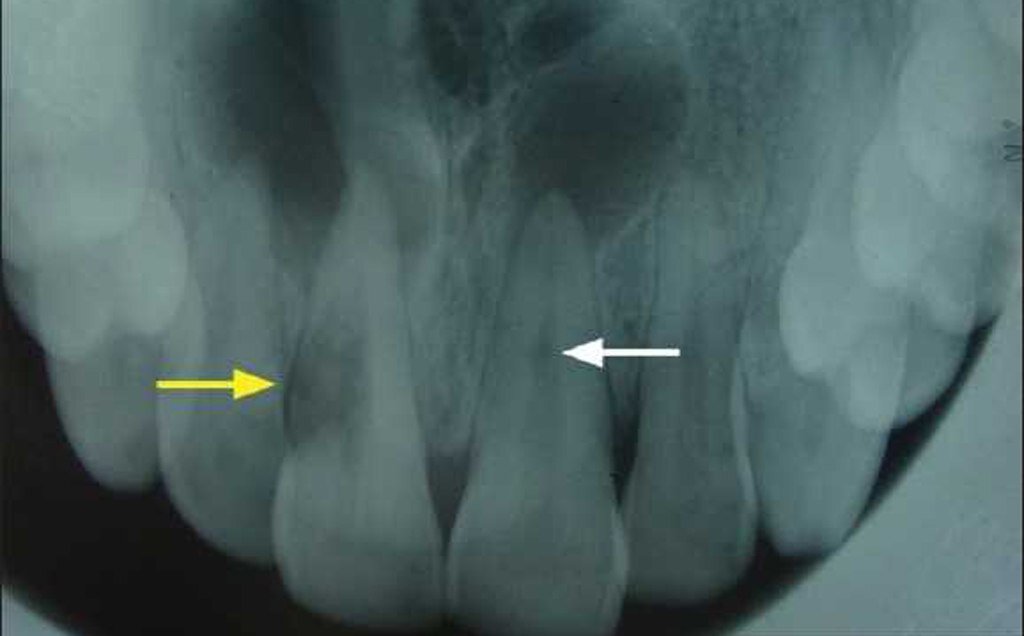
Figure 2. Root resorption.
The most common etiological prerequisites for cervical resorption can be identified as follows:
- improper application of orthodontic force,
- surgical intervention in the area of the alveolar bone ridge with disruption of the integrity of the tooth-gingival attachment,
- errors in performing the intrapulpal bleaching protocol,
- result of acute mechanical trauma to a specific tooth or the entire jaw.
Pathogenesis
The destruction of tooth tissue begins in the area of the root neck slightly below the level of the tooth-gingival attachment. Through a minor exposed area of tissue, the penetration of resorbing cells into the root dentin occurs. At the initial stage, the focus of resorption does not penetrate towards the pulp chamber, it spreads along the root surface due to the high protective characteristics of the predentin. Such a principle of progression of the pathological process inside the root wall is the reason why cervical resorption is also referred to as invasive or external-internal resorption.
Gradually, the resorption area expands and reaches the root canal. With prolonged progression, cervical resorption can also damage the adjacent alveolar bone, which lies next to the resorption lacunae. Radiologically, this process resembles a periodontal disease with the formation of a bone pocket.
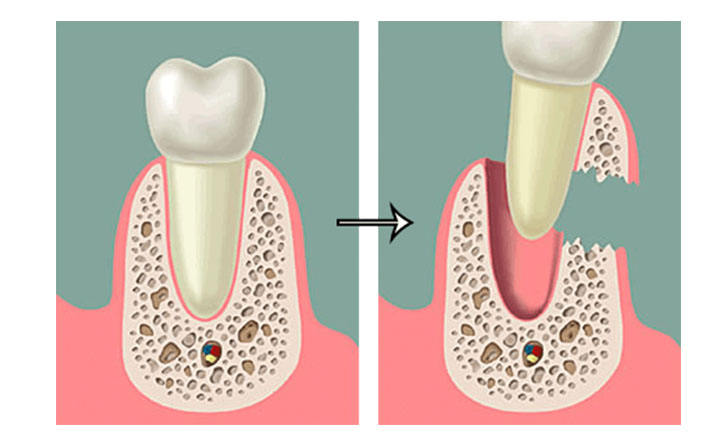
Figure 3. Involvement of bone tissue in resorption.
It is important to consider the fact that cervical resorption is not a reactive response of the pulp, therefore, its viability does not affect it. This explains the often asymptomatic progression of the disease, with detection occurring by chance.
Diagnosis
A tooth undergoing cervical resorption sometimes acquires a pinkish hue or a pink spot of varying intensity can be detected on its surface in the cervical area. This coloring is due to the translucency of the granulation tissue filling the resorption lacunae due to its abundant vascularization.
During the stage of differential diagnosis, it is necessary to remember the absence of disturbances from the pulp side: the results of electric pulp testing in cervical resorption and other tests for pulp vitality usually do not differ from normal indicators.
The progression of pathological processes of cervical resorption causes destruction of the crown, which may be accompanied by perforation of the pulp chamber. In such cases, during the collection of the patient's history, complaints of pulpitic pains are noted.
Clinical Manifestations
A common reason for a patient with existing cervical resorption to seek medical attention is a complaint about a change in the color of the affected tooth. The patient notes that the tooth has never been painful and there are no pain sensations at the time of examination. Electroodontodiagnostic indicators are within normal limits. Testing the tooth's response to thermal stimuli showed that the cold test confirmed the vitality of the pulp.
The patient's history sometimes includes a mechanical acute trauma, during which the tooth itself and the surrounding periodontal tissues were injured.
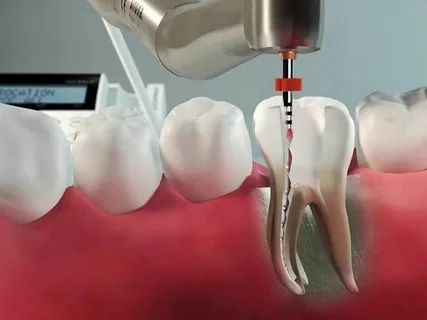
Figure 4. Endodontic treatment for pulp chamber perforation.
Radiologically, an extensive area of tooth tissue destruction is detected. Careful retraction of the soft tissues with a blunt smoother, which fill the defect on the crown surface, demonstrates that their growth originates from the periodontal tissues, not related to the pulp (differential diagnosis with pulp polyp).
The above diagnostic manipulations allow the diagnosis of cervical resorption.
Treatment Principles
The most effective treatment for cervical resorption involves the surgical removal of granulation tissue. Subsequently, the defect in the cervical area of the tooth is treated according to standard principles of cavity preparation for dental caries, which ensures reliable retention of the restorative material, restoring the lost anatomical shape of the tooth.
If the pathological process has reached the pulp chamber and perforation has occurred, endodontic treatment is necessary. Subsequently, to restore a tooth affected by cervical resorption complicated by pulp inflammation, an orthopedic construction will be required, as such a process proceeds with significant loss of tooth tissue.
Sequence of treatment stages
The overgrown tissue is surgically excised, optimally using a diathermocoagulator for this purpose. The removed fragment undergoes histological examination, the results of which indicate that it is a fragment of dense fibrous tissue, with focal lymphocytic infiltration, covered peripherally by a layer of non-keratinizing stratified squamous epithelium.
Next, the tooth is delicately dissected. However, despite the utmost care in dissection, after cleaning the cavity of affected tissues, communication with the pulp chamber may be detected, necessitating endodontic treatment of the tooth.
Upon completion of all therapeutic procedures, the tooth is subject to orthopedic restoration, it loses a significant volume of tissue, which leads to a high risk of fracture in the future. However, sometimes patients categorically refuse prosthetics, insisting on restoring the tooth with filling materials.
In such cases, it is possible to manufacture a post and core or to replenish the volume of lost tissues using a fiberglass post. Subsequently, the tooth crown is restored using a light-curing composite material.
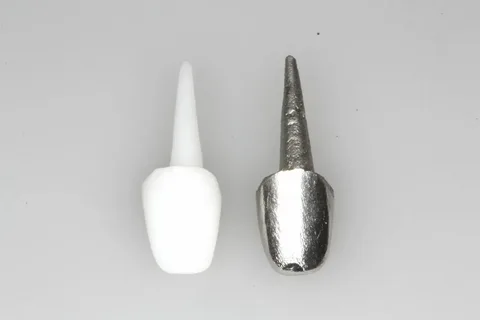
Figure 5. Cast post and core.
If a patient is diagnosed with initial cervical resorption during clinical examination, treatment may be postponed for some time, but the patient is put on clinical monitoring. If dynamic observation does not confirm the progression of the cervical resorption process, treatment is postponed again.
Summarizing the above, we conclude that cervical resorption is a pathology accompanied by damage to tooth tissues, which requires maximum attention from the dentist and extensive theoretical knowledge. Therapy for extensive cervical resorption requires a comprehensive approach, involving specialists of various profiles. After the treatment of cervical resorption, patients are recommended to undergo dynamic observation, which helps not only to assess the condition of the treated tooth but also the other teeth.
Clinical protocols for the treatment of invasive cervical resorption are presented at the webinar Interdisciplinary Treatment of Invasive Cervical Resorption.